What’s New!
Integrative Oncology: A Proven Model for Whole-Person Cancer Care
By Dr. Daniel Vicario, M.D., ABIHM
A Legacy of Innovation, Integrity and Healing
Over the past several months, I have reflected deeply on what it truly takes to create an optimal healing environment in cancer care, one that is clinically rigorous, evidence-informed, deeply compassionate and grounded in integrity. These reflections consistently bring me back to the integrative oncology model we built at the San Diego Cancer Center through the non-profit San Diego Cancer Research Institute (SDCRI).
What we created was not simply an adjunct program, but a fully integrated, state-of-the-art model of whole-person cancer care, one that remains relevant today and deserves to be studied, learned from and adapted globally…
Continue reading on the Letters from Dr. Daniel Vicario page.
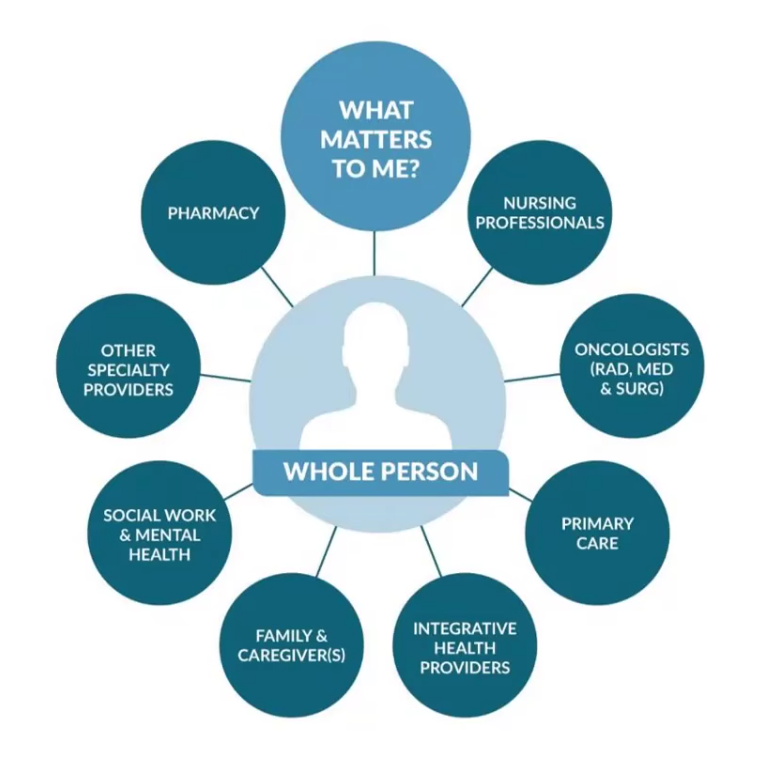 Whole Person Cancer Care & Integrative Oncology with Wayne Jonas, MD
Whole Person Cancer Care & Integrative Oncology with Wayne Jonas, MD
We are proud to bring attention to this video with Dr. Wayne Jonas!
Whole Person cancer care is a comprehensive approach that seeks to promote recovery and well-being while managing disease. The importance of what matters to the person guides treatment planning alongside what’s the matter. So the question is, are we using the right tools to actually help people heal?”
Watch it here.
Visit Dr. Wayne Jonas’s website: Healing Works Foundation
Genomic Oncology
 Dr. Mark Adler, Institute Director, heads the Genomic Oncology Diagnostics and Second Opinion Initiative, a new generation platform for developing treatments tailored to the individual patient. It involves the application of sensitive genomic tests to the determination of a tumor’s drug sensitivity and resistance. In addition, a person’s hereditary traits and a tumor’s genetic signature will be used to determine how best to eliminate a given cancer with a specific therapy or agent.
Dr. Mark Adler, Institute Director, heads the Genomic Oncology Diagnostics and Second Opinion Initiative, a new generation platform for developing treatments tailored to the individual patient. It involves the application of sensitive genomic tests to the determination of a tumor’s drug sensitivity and resistance. In addition, a person’s hereditary traits and a tumor’s genetic signature will be used to determine how best to eliminate a given cancer with a specific therapy or agent.
We have added 5 new articles authored by Dr. Adler to this page.
Read more here!
Understanding Cancer
Modern Biologic Principles Shaping Disease and Therapy
Dr. Adler’s new books is now available to read on PDF! This book is designed to be read in whatever order best serves the reader. Each section opens with a brief guide to help readers decide where to focus. Chapters can usually be read independently, and key terms are defined throughout. This book does not promise easy answers, but it aims to replace confusion with understanding, enabling more confident engagement with the decisions that cancer care requires.
Read it here!
Resource Highlights
We’ve recently added three new books to the Suggested Reading page:
The Resilience Mindset: How Adversity Can Strengthen Individuals, Teams, and Leaders by Terry Healy. An actionable framework to overcome adversity and create a more fulfilling life.
I Am with You: Love Letters to Cancer Patients by Nancy Novak. An anthology written by and for amazing cancer patients everywhere.
Surviving the Storm: A Workbook for Telling Your Cancer Story by Cheryl Krauter. This is a book for people who need to tell the story of how they’ve been touched by cancer.
Check out those and all the other wonderful books here.
A new section of Resources has been added just for Veterans. We salute our brothers, sisters, and siblings in service, and know that they need support just as much as anyone else. See those links here.
We have added a new resource: Helping Young Hearts Heal: A Guide To Grief Support for Children Children are often overlooked when a family is grieving over the loss of a loved one. This is an amazing guide to help children of all ages through their loss.
Go to our Resource Page for more.
Dr. Brenner’s Musings

#12 “How To Analyze Dreams & Unusual Life Experiences”
While we still mourn the passing of our beloved Dr. Paul Brenner, we can still enjoy the beautiful and inspiring words he shared with us over the years.
In this blog, Dr. Breener wrote about a beloved therapist and teacher who shared a simple yet profound practice for turning dreams and daily experiences into insight, meaning, and personal growth.
On his personal page is a summary of Dr. Brenner’s professional career.
Expressive Arts Therapy with Alessandra Colfi, Ph.D.
 – Expressive Arts Therapy and Yoga will engage attendees at 2026 National Symposium for Palliative Care June 4th & 5th, 2026 at CSUSM, San Marcos, CA
– Expressive Arts Therapy and Yoga will engage attendees at 2026 National Symposium for Palliative Care June 4th & 5th, 2026 at CSUSM, San Marcos, CA
Rooted in Compassion: A Collective Expressive Arts Garden
– Patients interested in creating together in live workshops can sign up for Alessandra’s spring 8-week series at UC San Diego Cancer Services ‘Metaphors from Nature’ starting April 3 through May 22 – an update with the link with details and to register will be provided.
– Join me in New Orleans for Expressive Arts Therapy and Yoga for Cancer Recovery at APOS Conference in March 2026 https://apos.societyconference.com/v2/
SDCRI will be present at APOS conference as a Community Partner, where you can join Dr. Alessandra Colfi
– Alessandra has written a new article on “Yoga for Supporting Students with Osteoporosis and Osteopenia”, and we’ve added an article section to the Expressive Arts page.
Check it all out right here!
– Alessandra is now offering a new Gentle Yoga class!
This class is open to all female cancer survivors; there is no fee to participate but interested participants are asked to complete 2 simple forms before joining in.
Learn more about that class here!
–Need CEs? Consider Healing Through Art: Discover the power of art to heal and transform in this 6-week, online professional development program which Alessandra teaches through CSUSM starting February 26. Earn 24 CE hours.
-There is plenty of evidence that exercise is the most effective lifestyle practice which improves quality of life and outcome in recovering from cancer and lowering risk of recurrence. However, many patients hold back for fear of getting hurt and don’t enjoy exercising… In order to support and encourage patients to exercise safely and join low-impact Zumba classes, Alessandra researched and wrote a new article: The Hidden Risks of Holding Back During Exercise
“For a short time, I taught a Zumba class on Zoom, recording in a small studio where I had to keep my movements tight and stay within a limited space to remain visible on camera. After just a couple of weeks, I began experiencing aches all over, especially in my hips and knees. That discomfort ultimately led me to stop teaching the class after a couple of months…” Read on here.
-Take a look at Alessandra’s page for project schedules along with registration information. Have a look here!
Mary’s Reality-Based Nutrition
Each one of us is a unique individual on our own unique path. One size does not fit all when it comes to personal healthcare. Therefore, it is important for us to be our own advocates when it comes to our health. The first step is educating yourself about your disease and the role nutrition plays in treating it. Take a look at my page for resources to help you improve your diet. Mary’s Reality-Based Nutrition
Follow me on my Facebook page for recipes: Check it out here! And you can follow me on Pinterest!
Videos and Talks
 Gregg Braden Invitational – CHI The Energy that Heals – This is a recent Zoom conversation regarding CHI Initiative’s upcoming documentary “The Energy that Heals”, and CHI’s “amazing ability to bring together diverse practitioners, thinkers, and actors with the goal of empowering individuals, societies, and humanity to build healthier societies and sustainable stewardship of our planet.”
Gregg Braden Invitational – CHI The Energy that Heals – This is a recent Zoom conversation regarding CHI Initiative’s upcoming documentary “The Energy that Heals”, and CHI’s “amazing ability to bring together diverse practitioners, thinkers, and actors with the goal of empowering individuals, societies, and humanity to build healthier societies and sustainable stewardship of our planet.”
Dr. Vicarios’s interaction starts at around minute 38. The documentary “The Energy that Heals” is under production. This is the link to CHI’s website with a recent Webinar that explains this exciting documentary project: https://www.chi.is/