SDCRI is inviting people, organizations, and companies in the Integrative Oncology & Integrative Therapies community to contribute articles to our Education page. We are very excited to be able to present these authors and hope that you enjoy what they have to share!
We have switched this page from monthly updates to updating when we find pertinent articles to post.
Here are the articles we have to offer today:
Acceptance, The Truest Definition of Love by Dr. Paul Brenner, posted on April 3rd, 2022
How to Keep Coronavirus Worries from Disrupting Your Sleep by Jill Suttie, published on berkley.edu on April 14th, 2020
The War on Cancer at 50: The Origin Begins With a Socialite Citizen-Lobbyist by Gabrielle Emanuel, published on medscape.com on January 06, 2022
We Are All Miracles by Dr. Paul Brenner, posted January 5th, 2022
Long-Term Expressive Art Therapy and Cancer Care by Alessandra Colfi, Ph.D., posted December 2nd, 2021
Feelings and Cancer by National Cancer Institute, last updated August 20, 2018
Can mRNA Vaccine Technology be Used to Treat Cancer? by Mary Hollander, R.N. and Daniel Vicario, M.D., posted on October 1st, 2021
Feeling Artsy? Here’s How Making Art Helps Your Brain an intro by Alessandra Colfi, Ph.D., posted September 3rd, 2021.
Scholarships and Support for College Students With Cancer & Cancer Survivors published by edubirdie.com on April 28th, 2021
The Greatest Invention Ever by Paul Brenner, M.D., Ph.D., posted July 1st, 2021
Socializing as COVID restrictions ease… let’s ease anxiety! by Alessandra Colfi, posted on June 1st, 2021
Be your own Cheerleader: a Compassionate, Encouraging Approach to Manage Stress by Alessandra Colfi, posted on May 1st, 2021
Every Organization Has A Story. Here’s Ours. by Dr. Andrea Deerheart with The HeartWay, shared on March 1st, 2021
Integrative Oncology Resources and Daily Ritual Summary, Checklist, and Reminders by Daniel Vicario, M.D., posted on February 1st, 2021
11 Questions to Ask About COVID-19 Research by Jeremy Adam Smith, EMiliana R. Simon-Thomas, published on greatergood.berkley.edu, December 16th, 2020
Medication management for cancer patients and caretakers by SINGLECARE TEAM, updated on November 5th, 2020
Hope Made Visible™, International: An ongoing journey by Alessandra Colfi, PhD, posted on November 2nd, 2020
Breathe Away Anxiety by Lisa Nicholson, posted on October 6th, 2020
Travel during the COVID-19 Pandemic from cdc.gov, posted on September 4th, 2020
Cold Flashes and Breast Cancer by Lisa Nicholson, posted on August 3rd, 2020
Depression in the time of Covid-19 by Paul Brenner, M.D., Ph.D, posted on May 19th, 2020
How Meditation Can Support Your Community and Wellbeing by Nina Fry-Kizler, MA, published on March 27, 2020
The Queen of Pandemics: Corona virus reflection and resources by Alessandra Colfi, PhD, posted on March 27th, 2020
Best Essential Oils 2020 on consumeradvocate.org, updated on February 1st, 2020
Featured Articles Archive 2019
Featured Articles Archive 2017-2018
Featured Articles Archive 2014-2016
Acceptance, The Truest Definition of Love
by Dr. Paul Brenner
Love is one of the most beautiful of words. It rolls off one’s lips and the “V” lingers into Infinity. Love has a plethora of meanings but let’s pull the honesty card. Love is a feeling. I have been thinking about this for a long time and convinced myself that love is the full acceptance of the moment. Merriam-Webster refers to love as affection, attraction, devotion, adoration, and so much more, but usually love is a feeling. I have had this need to bring this over-used word towards a tangible meaning. And this has led me to the understanding that love is the unconditional acceptance of what is in the moment.
I was first brought to this definition unconsciously by my mother. When I was a child and complained about something that happened to me the day before, she would casually say, “Paul, what was, was.” Or I came home and said, “I really need to go to Medical School and don’t know if I’ll ever get in.” And she would respond, “Honey, what will be will be.” Lastly, I would come home forlorn and tell her that I was just cut from baseball and minimally unconcerned, she would look at me and repeat for the hundredth time, “What is, is, my honey.” Over time, she drilled into me, what was, was; what will be, will be, and what is, is. She taught me to accept life in the moment, and then to choose what to do in the next moment. I can either stay in that evolving moment or change how I want to experience it, but don’t complain about life. Love is the acceptance of unfolding life, from minute to minute.
I was recently asked to meditate on sending love to Ukraine. I thought the best way I could help the people of Ukraine was to accept that they are in a horrific war not of their choosing. All I could do is first accept what was going on and then ask myself how I may best respond to the Ukrainians in ending the war. I would imagine if I were in a group sending love to the Ukrainians, we would all be sending what each one of us thought was our own definition of love. What they need in that moment was food, clothing, ammunition, participation, not my love, but my giving in whatever tangible way I can meet their needs. Where and when I can accept another where they are and what brought them to their understanding of the present moment is love. The unconditional acceptance of another’s moment in life, is an act of love. Do I accept Putin’s moment to restore the Russian Dynasty of the past? Yes, until it becomes destructive. At that moment, my acceptance turns to distrust and avoidance. Acceptance is not a constant. Acceptance is a moment-to-moment decision of how to love and participate in life.
About Dr. Brenner
Featured Articles Archive 2017-2018
Back to the top.
How to Keep Coronavirus Worries from Disrupting Your Sleep
by Jill Suttie
A sleep expert weighs in on how to get a better night’s rest during this time of heightened stress.
Many people I know have been complaining lately about losing sleep. It’s no surprise why. All of us are feeling increased stress and worry, and experiencing changes in our work and family life. The novel coronavirus can keep us up at night.
What can we do to protect our sleep during this time? For answers, I turned to Shelby Harris, the former director of the Behavioral Sleep Medicine Program at Montefiore Medical Center, an associate professor at the Albert Einstein College of Medicine, and author of the book The Women’s Guide to Overcoming Insomnia. We discussed what’s driving sleep disruption, the place of news and social media in our lives, the best way to binge your favorite TV shows, and more.
Jill Suttie: Why do you think it’s important to consider our sleep during a time like this, when so much else is going on?

Shelby Harris: Sleep is important for so many things. It’s important for mood regulation, emotion regulation, as well as the immune system. We need sleep to keep us as sane as we can be and also to keep ourselves healthy.
Also, it’s important for our relationships. People who are sleep-deprived tend to be more irritable with their family and more irritable at work. We’re already stressed to begin with, but without enough sleep, people will lash out a lot easier and a lot quicker at others around them. Our irritability goes from zero to 60 a lot faster when we are sleep-deprived.
JS: People seem particularly anxious right now. Is this playing a role in sleep disruption? Are other things contributing?
SH: People are definitely worried right now. They’re worried about their families, about money, about what’s going on in the world. And even people who aren’t typically anxious are now saying that their brains are so busy that they can’t turn them off to go to sleep. Or they wake up two hours later and their brain is just right there thinking about news and about life, and they just can’t quiet it down.
But there are also people who know that their families are fine, and while they’re concerned about the world, they’re not overly worried. What gets them off track with sleep is the lack of a schedule, the lack of routine in their lives. They’re not in their same beds, or they’re not going to sleep and waking up at the same time. Maybe they’re watching the news and getting bright-light exposure at night, or they’re not exercising the same way they used to, or they’re not socializing during the day. When their routine is taken away from them, that’s when people get thrown off their sleep.
JS: How does not socializing affect our sleep?
SH: When I think of socializing, I think it’s like charging your battery. It’s not about just talking to people over Zoom, but about people having a lunch date or working out with a partner and going out for a walk together. These are all ways to help bolster your mood by socializing, but they also mean you’re getting light exposure, which charges your battery.
If we’re not doing those things—if we’re not connecting with people and we’re not going out of the house—it’s just going to make it harder for us to sleep at night. Plus, if people feel more isolated, that can negatively impact their mood, too.
JS: You mention watching the news as a problem, but we need to stay informed.
SH: I’m a huge fan of limiting your news intake, and I think everyone needs to stop checking the news at night, when nothing is changing. People should try to check news no more than once a day, if that. And people need to be very thoughtful about what they’re checking and why they’re checking it. Here in New York, I’m having people just watch Governor Cuomo’s conference briefing every day, because it’s really the least triggering source of news for people.
JS: Do you think that positive or inspiring news could be useful now?
SH: It can be, but staying away from all news at night is a good idea. Not that you should live in avoidance—that’s not good either. But, at night, you just need to find a way to wind down. Maybe you could add some positive news into your hour or half hour of news during the day. But at nighttime, that’s when you should practice gratitude, practice meditation, practice the stuff that’s more personal to yourself.
JS: I’m hearing people complain about three different sleep problems: not being able to fall asleep, waking up in the night feeling panicky, and waking up too early without a full night’s sleep. Do you see those as separate problems requiring different interventions? Or are they all the same problem?
SH: I can’t really say, because people’s sleep problems are so varied. Sometimes depression can cause early-morning awakening, but so can anxiety. Then again, a busy brain can be the cause of us having trouble falling asleep. A lot of women who’re going through perimenopause and hormonal issues can wake up in the middle of the night, or so can people with sleep apnea or diabetes. So, it’s hard to make blanket statements—there are so many different factors that can cause these things.
Even so, I tend to treat them all very similarly. I try to have patients practice limiting time in bed if they’re not sleeping. If you’re not sleeping, you shouldn’t be in bed. And you shouldn’t try to force sleep—that’s the worst thing you can do.
I’m encouraging people to use meditation a lot during the day, because that helps with all of these sleep issues—at the beginning of the night, the middle of the night, and the early-morning awakenings.
Also, some people may tell you that if you didn’t sleep at night, you should take a nap during the day to compensate for the loss of sleep at night, or to sleep in late in the morning, or to go to bed earlier than usual. But that’s all stuff that’s actually going to make it worse. So, I recommend people keep a stricter sleep schedule when they’re not sleeping well.
A lot of these recommendations help across the board, but what I might change is the timing of going to bed—for some people. I might have some people stay up later to push their wake time later; but that’s very individual and varies based upon their sleep schedule and how severe the problem is. It depends if someone’s waking up super early—like two in the morning every night.
JS: A lot of my friends have been sharing great TV shows and movies to stream or watch at the end of their workday. Is watching these a problem for sleep?
SH: It’s fine and not fine. People will binge-watch in a good way—maybe to get out of their reality. But then they lose track of what time it is and, before they know it, it’s an hour or two or three later than when they should be going to bed. So, what I usually recommend people do is to watch one show and then turn off the auto function on Netflix (or whatever service it is) so that when the show ends, you make a mental note of looking at the time. If it’s close to your bedtime, you turn off the show. People need to stay away from screens at least the half hour to an hour before bedtime, because that bright light really does delay sleep.
JS: What about the content of the show? Does that make any difference?
SH: Light actually has a bigger influence than content. That’s why they make a huge deal in the sleep field about blue-light exposure before bed and during the night. But yeah, of course what you watch is going to make a difference, too.
That being said, I’ve worked with a lot of millennials over the years who were watching The Office and Friends—I don’t know why those two shows, but they love those two shows—and they will not change to become a reader. So, what I have them do is use blue-light-blocking glasses that you can get online to watch TV. That’s worked for them, because those shows are calming and funny and the glasses block most of the blue light.
I haven’t seen content make a big difference. As long as it takes you out of stress, it’s fine. But I am a big fan of just old-school methods for calming your mind before bed. Find a book, find a magazine or a puzzle if you can. Up until an hour before bed, you can watch all the TV you want. But, from a sleep preservation standpoint, you don’t want blue light right before bed, because it reduces your natural melatonin. Melatonin is the hormone usually released in your brain when the sun goes down and makes you sleepy. Interfering with its release is a terrible idea.
JS: Is there anything else that you think we need to know to sleep better?
SH: Some people need to stay away from social media as much as possible. I want people to connect, but some social media feeds tend to be triggering for people.
Having a routine is key, because if you don’t have routine during the day, you’re not going to have any routine at night. Too many people are working into the late-night hours, because they can’t keep ahead of everything. They need to try to set a cutoff time—a strict bedtime and wake time—and to really end their day so that they reduce white-light exposure at night.
Also, make sure when you’re working during the day that you have bright light. Open your shades, even if it’s cloudy out—especially when you first wake up in the morning. Then, an hour or two before bed, start dimming the light, to say to your brain that it’s bedtime now. You should get into a rhythm where it’s light during the day and dark at night, to help set your nighttime circadian rhythm. That will help you sleep, too.
This article originally appeared on Greater Good, the online magazine of the Greater Good Science Center at UC Berkeley.
The War on Cancer at 50: The Origin Begins With a Socialite Citizen-Lobbyist
by Gabrielle Emanuel, WBUR
Our Featured Article for February is a fascinating history and timeline of how and when the decision to invest in cancer research took hold thanks to passionate activism, political pressure, and philanthropy. It all began with the indignation of a 4-year-old little girl named Mary. Mary Lasker carried with her the memory of that day when she visited a woman with breast cancer. Even at that young age, she recognized the unbearable suffering and the limited medical care for the treatment of cancer. This article tells her story of bringing this lack of care and research into the cause and treatment of cancer to the public and the politicians of the day.
Not only do we owe this wonderful activist and philanthropist our gratitude for the progress in the treatment of cancer but it is also worth noting that we have come a long way in regard to the stigma and burden carried by patients and families.
Click the link below.
Medscape: The War on Cancer at 50: The Origin Begins With a Socialite Citizen-Lobbyist. By Gabrielle Emanuel, WBR, January 6, 2022.
We Are All Miracles
By Dr. Paul Brenner
The sheer gift of LIFE IS A Miracle. If you could think, but for a moment: all the combinations and permutations that made you, you, is simply a miracle beyond belief or words. Two microscopic cells fused and divided, replicated forty-one times, to create millions of cells with special DNA, emotions, understanding, and beliefs; unlike any other human that has ever been created. Even identical twins, within a minuscule time, become different; as their epigenetic experiences begin to differ, and change what was once similar to different. You’re a miracle, a one-of-a-kind, who has forever imprinted the history of humankind with your uniqueness. Your value has no price. There will never be another as you. You’re irreplaceable. And, have you ever said, “Thank you,” for your unique you?
Why you? Why have you been chosen to love and experience a life that no other person has ever or ever will be able to experience again? This miracle carries with it only one downside: loneliness. No other can ever truly know you or be you. Yes, you are a Miracle, as are others; and love others for they share in your loneliness. Please cherish your uniqueness, and understand the truth of loneliness as all-oneness. If you want to see a miracle, look in the mirror. Be kind to all the other Miracles in your life, who never knew that you were also a lonely Miracle.
About Dr. Brenner
Back to the top.
Long-Term Expressive Art Therapy and Cancer Care
By Alessandra Colfi
An excellent article in the Journal of Clinical Oncology, supporting significant benefits for cancer patients involved in a long-term Expressive Art Therapy program, has come to our attention. The article confirms that safety, togetherness, shared circumstances, freedom and confidence are as much a part of the healing power as the art expression itself. The benefits transcend the immediate expression and over time, they bring participants to cultivate and experience equanimity, agency, resilience, confidence and spill over into interpersonal relationships and life’s purpose.
It is ground-breaking that the authors not only surveyed participants according to a rubric but also engaged patients with open-ended reflections which resulted in patients’ personal narratives. According to the Journal, these narratives support the success of the study.
The study is encouraging oncologists to recommend and even refer patients to long-term art therapy programs, and that cancer centers should provide longer-term expressive arts therapy programs for their patients.
This article and study provide validation of the healing benefits of community-based, long-term expressive arts therapy in patient-centered, integrated medical care, supporting implementation, engagement, and access for patients.
With deep gratitude to our leadership at San Diego Cancer Research Institute for welcoming and supporting the Expressive Arts Therapy program starting in 2009 and for facilitating its continuation and expansion to this day!
Patients and caregivers interested in learning more and participating in the Expressive Arts Therapy program, please contact the facilitator Alessandra Colfi, Ph.D.,
Alessandra@AlessandraColfi.com ~ 858.735.5708
Reference:
Developing a Community for Patients With Cancer Through Longer-Term Art Therapy | JCO Oncology Practice (ascopubs.org), Vol. 17, Issue 4. By Sam Brondfield, MD,
MAEd1; Naike Bochatay, PhD2; and Cynthia Perlis, BS, MFA3
Feelings and Cancer
National Cancer Institute, National Institute of Health
 Just as cancer affects your physical health, it can bring up a wide range of feelings you’re not used to dealing with. It can also make existing feelings seem more intense. They may change daily, hourly, or even minute to minute. This is true whether you’re currently in treatment, done with treatment, or a friend or family member. These feelings are all normal.
Just as cancer affects your physical health, it can bring up a wide range of feelings you’re not used to dealing with. It can also make existing feelings seem more intense. They may change daily, hourly, or even minute to minute. This is true whether you’re currently in treatment, done with treatment, or a friend or family member. These feelings are all normal.
Often the values you grew up with affect how you think about and cope with cancer. For example some people:
- Feel they have to be strong and protect their friends and families
- Seek support and turn to loved ones or other cancer survivors
- Ask for help from counselors or other professionals
- Turn to their faith to help them cope
Whatever you decide, it’s important to do what’s right for you and not to compare yourself with others. Your friends and family members may share some of the same feelings. If you feel comfortable, share this information with them.
Young people with cancer can also learn more on the Emotional Support for Young People with Cancer page.
Stress and Anxiety
Both during and after treatment, it’s normal to have stress over all the life changes you are going through. Anxiety means you have extra worry, can’t relax, and feel tense. You may notice that:
- Your heart beats faster.
- You have headaches or muscle pains.
- You don’t feel like eating. Or you eat more.
- You feel sick to your stomach or have diarrhea.
- You feel shaky, weak, or dizzy.
- You have a tight feeling in your throat and chest.
- You sleep too much or too little.
- You find it hard to concentrate.
If you have any of these feelings, talk to your doctor. Though they are common signs of stress, you will want to make sure they aren’t due to medicines or treatment.
Stress can keep your body from healing as well as it should.
If you’re worried about your stress, ask your doctor to suggest a counselor for you to talk to. You could also take a class that teaches ways to deal with stress. The key is to find ways to control your stress and not to let it control you.
Sadness and Depression
Many people with cancer feel sad. They feel a sense of loss of their health, and the life they had before they learned they had the disease. Even when you’re done with treatment, you may still feel sad. This is a normal response to any serious illness. It may take time to work through and accept all the changes that are taking place.
When you’re sad, you may have very little energy, feel tired, or not want to eat. For some, these feelings go away or lessen over time. But for others, these emotions can become stronger. The painful feelings don’t get any better, and they get in the way of daily life. This may be a medical condition called depression. For some, cancer treatment may have added to this problem by changing the way the brain works.
Getting Help for Depression
Depression can be treated. Below are common signs of depression. If you have any of the following signs for more than 2 weeks, talk to your doctor about treatment. Be aware that some of these symptoms could be due to physical problems, so it’s important to talk about them with your doctor.
Emotional signs:
- Feelings of sadness that don’t go away
- Feeling emotionally numb
- Feeling nervous or shaky
- Having a sense of guilt or feeling unworthy
- Feeling helpless or hopeless, as if life has no meaning
- Feeling short-tempered, moody
- Having a hard time concentrating, feeling scatterbrained
- Crying for long periods of time or many times each day
- Focusing on worries and problems
- No interest in the hobbies and activities you used to enjoy
- Finding it hard to enjoy everyday things, such as food or being with family and friends
- Thinking about hurting yourself
- Thoughts about killing yourself
Body changes:
- Unintended weight gain or loss not due to illness or treatment
- Sleep problems, such as not being able to sleep, having nightmares, or sleeping too much
- Racing heart, dry mouth, increased perspiration, upset stomach, diarrhea
- Changes in energy level
- Fatigue that doesn’t go away
- Headaches, other aches and pains
If your doctor thinks that you suffer from depression, he or she may give you medicine to help you feel less tense. Or, he or she may refer you to other experts. Don’t feel that you should have to control these feelings on your own. Getting the help you need is important for your life and your health.
Guilt
If you feel guilty, know that many people with cancer feel this way. You may blame yourself for upsetting the people you love, or worry that you’re a burden in some way. Or, you may envy other people’s good health and be ashamed of this feeling. You might even blame yourself for lifestyle choices that you think could have led to your cancer.
These feelings are all very common. It may help you to share them with someone. Let your doctor know if you would like to talk with a counselor or go to a support group.
“When I start to feel guilty that I caused my illness, I think of how little kids get cancer. That makes me realize that cancer can just happen. It isn’t my fault.” ~ Becky
Loneliness
People with cancer often feel lonely or distant from others. This may be for a number of reasons:
- Friends sometimes have a hard time dealing with cancer and may not visit or call you.
- You may feel too sick to take part in the hobbies and activities you used to enjoy.
- Sometimes, even when you’re with people you care about, you may feel that no one understands what you’re going through.
It’s also normal to feel alone after treatment. You may miss the support you got from your health care team. Many people have a sense that their safety net has been pulled away, and they get less attention. It’s common to still feel cut off from certain friends or family members. Some of them may think that now that treatment is over, you will be back to normal soon, even though this may not be true. Others may want to help but don’t know how.
Look for emotional support in different ways. It could help you to talk to other people who have cancer or to join a support group. Or, you may feel better talking only to a close friend or family member, or counselor, or a member of your faith or spiritual community. Do what feels right for you.
Gratitude
Some people see their cancer as a “wake-up call.” They realize the importance of enjoying the little things in life. They go places they’ve never been. They finish projects they had started but put aside. They spend more time with friends and family. They mend broken relationships.
It may be hard at first, but you can find joy in your life if you have cancer. Pay attention to the things you do each day that make you smile. They can be as simple as drinking a good cup of coffee, being with a child, or talking to a friend.
You can also do things that are more special to you, like being in nature or praying in a place that has meaning for you. Or, it could be playing a sport you love or cooking a good meal. Whatever you choose, embrace the things that bring you joy when you can.
Ways to Cope with Your Emotions
Express Your Feelings
People have found that when they express strong feelings like anger or sadness, they’re more able to let go of them. Some sort out their feelings by talking to friends or family, other cancer survivors, a support group, or a counselor. But even if you prefer not to discuss your cancer with others, you can still sort out your feelings by thinking about them or writing them down.
Look for the Positive
Sometimes this means looking for the good even in a bad time or trying to be hopeful instead of thinking the worst. Try to use your energy to focus on wellness and what you can do now to stay as healthy as possible.
Don’t Blame Yourself for Your Cancer
Some people believe that they got cancer because of something they did or did not do. But scientists don’t know why one person gets cancer and one person doesn’t. All bodies are different. Remember, cancer can happen to anyone.
Don’t Try to Be Upbeat If You’re Not
Many people say they want to have the freedom to give in to their feelings sometimes. As one woman said, “When it gets really bad, I just tell my family I’m having a bad cancer day and go upstairs and crawl into bed.”
You Choose When to Talk about Your Cancer
It can be hard for people to know how to talk to you about your cancer. Often loved ones mean well, but they don’t know what to say or how to act. You can make them feel more at ease by asking them what they think or how they feel.
Find Ways to Help Yourself Relax
Whatever activity helps you unwind, you should take some time to do it. Meditation, guided imagery, and relaxation exercises are just a few ways that have been shown to help others; these may help you relax when you feel worried.
Be as Active as You Can
Getting out of the house and doing something can help you focus on other things besides cancer and the worries it brings. Exercise or gentle yoga and stretching can help too.
Look for Things You Enjoy
You may like hobbies such as woodworking, photography, reading, or crafts. Or find creative outlets such as art, movies, music, or dance.
Look at What You Can Control
Some people say that putting their lives in order helps. Being involved in your health care, keeping your appointments, and making changes in your lifestyle are among the things you can control. Even setting a daily schedule can give you a sense of control. And while no one can control every thought, some say that they try not to dwell on the fearful ones, but instead, do what they can to enjoy the positive parts of life.
Can mRNA Vaccine Technology be Used to Treat Cancer?
by Mary Hollander, R.N. and Daniel Vicario, M.D.
In 2005 scientists at the University of Pennsylvania discovered mRNA. That’s right, it isn’t a new technology or an experimental technology. Research during the past two decades has led us to the COVID-19 mRNA vaccine from Pfizer & Moderna. The “m” in mRNA stands for messenger. The perfect name for it. The RNA is sent to our cells with a code that teaches our immune system to produce antibodies that will fight and destroy specific dangerous viruses. As the virus mutates, our immune system can now adapt itself to go after new variants as well. All this is thanks to the research started in 2005!
How does this relate to a new treatment for cancer? First, we must thank 2 scientists. They received the Nobel Prize for Chemistry in 2020. Take a look at the synopsis of their work; Jennifer A. Doudna and Emmanuelle Charpentier
Next, let’s look at two articles about how mRNA is being researched for use in cancer treatments. This first article is rather important because not only have researchers at MD Anderson been working with mRNA vaccines to treat cancer, they are already in Phase II clinical trials!
MD Anderson Cancer Center: Can mRNA vaccines be used in cancer care? By Devon Carter, January 25, 2021, “The COVID-19 vaccines mark the first widespread use of mRNA technology. They work by using synthetic genetic code to instruct the patient’s cells to recognize the coronavirus and activate the immune system against the virus.
But researchers began exploring how to use mRNA vaccines as a new way to treat cancer long before this technology was used against the coronavirus.”
“We’ve known about this technology for a long time, well before COVID-19,” says Van Morris, M.D. Here, he explains how mRNA vaccines work and how a team of MD Anderson colorectal cancer experts led by Scott Kopetz, M.D., Ph.D., are testing the technology in a Phase II clinical trial.”
Pancreatic cancer is difficult to treat. In those who survived for years after diagnosis, it was seen that their immune system kept cancer from returning. In the following article, Memorial Sloan Kettering researchers have been studying the use of an mRNA vaccine to treat pancreatic cancer & have moved into the clinical trial stage.
Memorial Sloan Kettering Cancer Center: Can mRNA Vaccines Fight Pancreatic Cancer? MSK Clinical Researchers Are Trying to Find Out, Tuesday, July 6, 2021 “Messenger RNA (mRNA) vaccines may be the hottest thing in science now as they help turn the tide against COVID-19. But even before the pandemic began, Memorial Sloan Kettering researchers had already been working to use mRNA vaccine technology to treat cancer.
Vinod Balachandran a physician-scientist affiliated with the David M. Rubenstein Center for Pancreatic Cancer Research and a member of the Human Oncology and Pathogenesis Program and the Parker Institute for Cancer Immunotherapy, explain how a collaboration with BioNTech — which developed the Pfizer-BioNTech COVID-19 vaccine — has led to a potential treatment for pancreatic cancer now in clinical trials.”
As you can see. mRNA technology has been around for decades. It holds the promise of new treatments for oncology and genetic diseases. It also opens the door to researchers for new scientific discoveries in medicine and agriculture.
If you are interested in how the process of getting a vaccine from research to approval, the CDC has a page with that information: Overview, History, and How the Safety Process Works.
With Warm Regards to our SDCRI community,
Mary Hollander, R.N.
Daniel Vicario, M.D.
Feeling Artsy? Here’s How Making Art Helps Your Brain
Introduction to the article by Alessandra Colfi, Ph.D.
During one of the most challenging times like facing a cancer diagnosis and the long and uncertain healing journey, losses, and the anxiety that often is experienced, looking for meaning and having the opportunity to create meaning brings healing, fosters resilience, and a renewed sense of purpose. How the experiences are processed is very important and can lead to Post-Traumatic Growth, which might include a change in perspective, appreciation for life, greater compassion, deeper spiritual awareness, a sense of peace and acceptance, and creativity, as the ability to see new possibilities. Creativity can be encouraged as a self-directed activity like doodling, coloring, sketching, gardening, cooking, moving to music, or joining an expressive arts weekly group that provides skillful guidance, safety, and inspiration to be engaged in processing those very challenging experiences and meaning-making.
Art can help us relax, find joy in playing and exploring, find a mindful focus as an anchor, help express our thoughts, and can help us reflect, generate purpose, and contain new ideas and make decisions. The symbolic quality of art-making helps to view experiences and changes as part of life’s journey and to create a sense of control over the circumstances that lie ahead.
Depending on your circumstances, consider joining one of these free offerings:
- Expressive Arts Therapy series ‘Metaphors from Nature: Awareness, Self-expression, Wisdom, and Nurturing’, facilitated by Alessandra Colfi, Ph.D. Choose Mondays 4 pm to 6 pm, or Fridays 10.30 am to 12.30 pm in September (no class 9/6, Labor Day). Offered via Zoom, it is free for cancer patients and caregivers.
Keeping Nature as a connecting thread, you’ll be playing and learning together, adding an artful dimension, and embodied mindful awareness for personal self-exploration and self-expression. PM @AlessandraColfi with your questions and to RSVP. - With compassion and caring support, Alessandra Colfi is also inviting those who are experiencing grief from loss to join in a weekly Expressive Arts series Healing Grief Thru HeArt. Thanks to the generous support of The HeartWay: Embracing Life thru Honoring Death this program is provided at no cost.
FREE SESSIONS on Saturdays 11 am – 1 pm.
September 11 through October 16, 2021, in Encinitas, CA
Facilitated by Alessandra Colfi, Ph.D., RYT-200. Contact her at: 858.735.5708 or Alessandra@AlessandraColfi.com for more information.
No Previous Art Experience is Required to Participate; a commitment to attend all 6 sessions is requested.
Safe COVID-19 protocol per CDC guidelines is followed.
Read the full article by Malaka Gharib on the NPR.org site!
Scholarships and Support for College Students With Cancer & Cancer Survivors
published by edubirdie.com

“The most disturbing aspect of dealing with cancer is the battle of both physical and mental factors that always come into play. The list of challenges that students face at each stage of cancer treatment is enormous because each person battling cancer is different and the reactions to chemotherapy or any other type of treatment will differ, making it hard to concentrate or sit through the lengthy lecture.”
Continue reading this article on the EduBirdie website.
The Greatest Invention Ever
By Paul Brenner, M.D., Ph.D.
I honestly believe that humans will always be able to accomplish more than technology. The human being, over generations, has within him/herself the ability to accomplish anything that can be imagined. This would be such things as teleportation, self-healing, and the ability to have instant knowledge. Instant knowledge will be within the grasp of all human beings, as will the inherent awareness of what is needed to serve LIFE in the future. Presently, humankind is limited only by its belief of what is possible.
An example can be seen in individuals as they tackle Parkour. The split-second decision-making that is required for Parkour seems to be astounding, but it is just the beginning. In my brief 87 year lifetime, I have seen individuals progressively run faster, think faster, learn faster, etc.; as if time and space have collapsed. We know the unborn can learn in-utero. The average IQ increases approximately three points a decade, and I imagine even this will be extended over time.
If we can change the dogma [beliefs] of what a human being’s limitations are in such as, IQ and bodily accomplishments; then we can begin the journey towards limitlessness. The rate at which children currently learn to master computers is remarkable. This is matched by the agility that some four or five-year-olds have on a skateboard; and the speed, agility, and mental awareness that allows adolescents to run and climb obstacles, requiring split-second decision making, simply by visualizing the feat beforehand.
Over time, these abilities – that now seem unbelievable – will be integrated into everyday tasks in the future. As we gradually learn that the body~mind is limitless, the collective consciousness that surrounds us will become more available to us. The collective consciousness will move us into direct knowing. The age of learning outside ourselves will no longer be required. What was once called intuition will rightfully be called, ‘direct knowing.’ The space that surrounds us is an extension of ourselves, and becomes available to those with the intention to serve LIFE.
At such a time, humankind will be able to achieve anything that it imagines; and will be of service to LIFE and the COLLECTIVE CONSCIOUSNESS.
Socializing as COVID restrictions ease… let’s ease anxiety!
By Alessandra Colfi, PhD, RYT-200, ZIN
Among the keywords that have become a part of most conversations for the past 15 months are precautions, restrictions, and anxiety. If we have been paying attention at all, we have noticed how our lives are interconnected and how interdependence works. There is a renewed sense of social responsibility, responsibility in our relationship and interactions with nature, how framing issues matters, how strong we feel about not going back to ‘the way many things were’.
Most people I talk to, and especially the most vulnerable patients, have worked hard to adjust mentally and physically to all kinds of restrictions and limitations, even to complete isolation; some people might have found it quite comfortable to stay home, Zoom or not, and get everything delivered. Most people, though, have been missing social interactions, hugs, spontaneity, even to the point of experiencing severe anxiety and depression, lacking the opportunities for emotional co-regulation.
Like a new dawn, many among us feel relieved, cautiously excited, but anxious about the newly recovered freedom, a sense of having choices again to resume in-person social interactions and travels.
There are no one-size-fits-all guides to what new freedoms the newly vaccinated should enjoy. We need to be aware that our bodies (as in body/mind/spirit/energy) have taken a long time to learn and adjust to isolation and will take some time to un-learn and adjust our behavior to in-person social interactions and trust those around us. Our brains are wired for connection, but the trauma generated by the pandemic rewired us for self-preservation.
At first seeing a lot of people at the grocery store or in the park might feel overwhelming, even more so at a backyard party or sporting event; gathering with friends and family calls for closeness, hugs, etc. Even small talk can feel awkward at first.
If anxiety arise, in any form, from a general sense of discomfort to shallow breathing, increased heart rate, or feeling lightheaded, start by simply taking slow breaths in and even slower outbreaths to self-regulate by activating the Parasympathetic Nervous System through the Vagus nerve; by doing so, the anxious brain in ‘fight or flight’ mode receives a message of safety and comfort which brings the whole body back to a baseline ‘rest and digest’ state.
If there is a specific area of the body that feels tight, like the solar plexus or chest, gently placing one hand on it and breathing slowly is comforting and it communicates safety and acceptance. Using one hand or both, gently squeeze each arm and each leg to ground and comfort yourself and regain a sense of calm control. Especially comforting is to give yourself a hug by crossing the arms and holding your shoulders with your hands.
One way to avoid feeling overwhelmed is to start meeting with just a few trusted people, who share the same understanding of safety, risk-factor, and precautions; it will likely make for more intimate and meaningful conversations. Instead of asking ‘are you vaccinated?’ opt for a friendly ‘Can I give you a hug?’ Just like it has been uncomfortable to be the ‘mask police’ it is just as uncomfortable to ask everyone we meet if they are fully vaccinated or not.
If you do feel a strong anxiety response in social situations or even as you get ready to walk out the door or into your friends’ backyard, something like what we commonly call a ‘panic attack’, there might be an association to previous incidents in which fear, pain, trauma had occurred, very likely a form of PTSD.
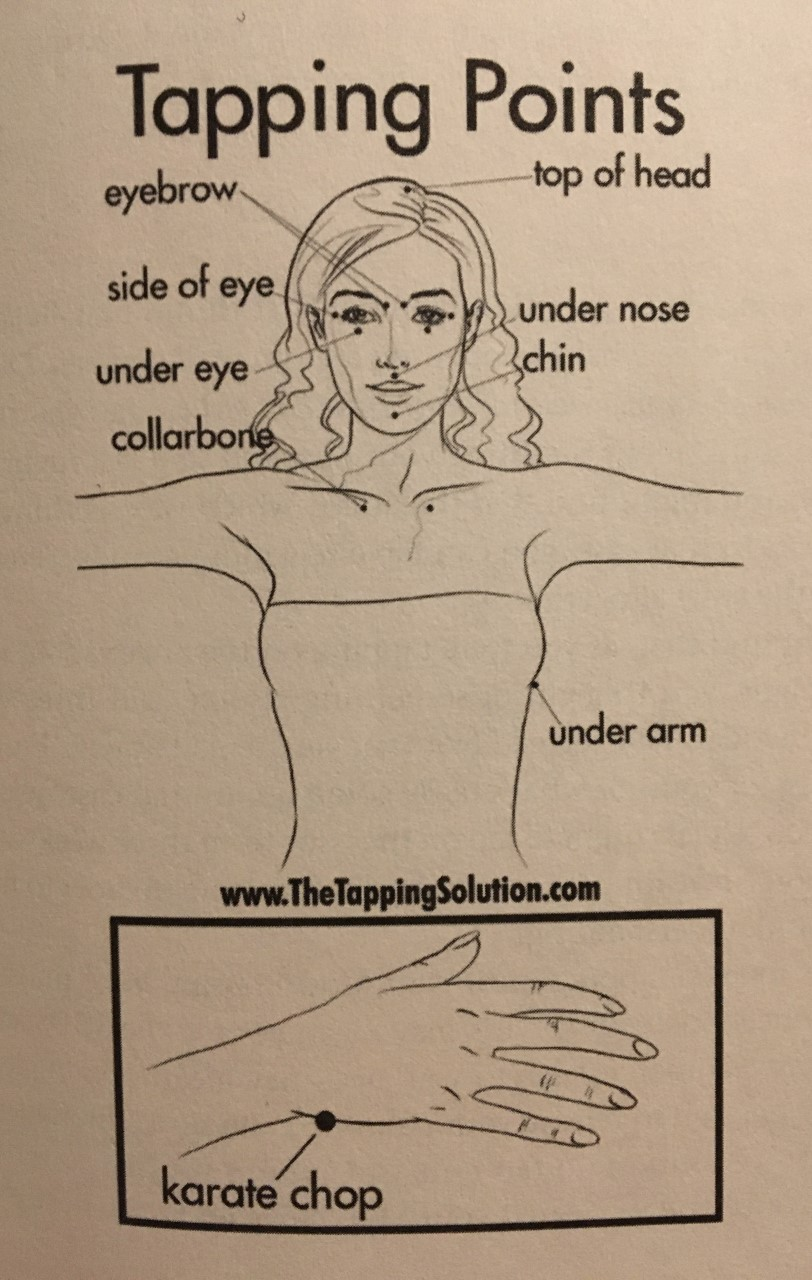
While professional help might be recommended or necessary, a very easy and effective tool to keep in your ‘bag of tricks’ is the Emotional Freedom Technique (EFT), known as tapping on acupressure points.
Tapping with your fingers on acupressure points connected along the meridians decreases activity in the amygdala and deactivates the ‘fight or flight’ response to a safe, calming ‘rest and digest’.
EFT can be a powerful tool especially in individual sessions with the integration of recalling and processing each stressful event, with safety and trust.
Time, patience, and compassion are necessary to ease ourselves into a big shift once again. We need to trust our ability to adapt; curiosity and flexibility will once again be key to resilience and let’s not forget that we are all in this together.
Hope this helps! For more information and techniques to help ease stress and anxiety contact Alessandra Colfi at Alessandra@AlessandraColfi.com or 858.735.5708.
Be your own Cheerleader: a Compassionate, Encouraging Approach to Manage Stress
By Alessandra Colfi, PhD, RYT-200, ZIN
Feeling stressed and overwhelmed from time to time is absolutely normal; we all experience such feelings when life’s demands overcome our perceived or objective capacity – in terms of time, strength, mental or emotional space, skills, and support from others.
Stress can also be layered with anxiety, especially when uncertainty about future outcomes dominates our thoughts. To some degree, we have all been feeling anxious since we found ourselves trapped in the global pandemic, afraid of getting sick with Covid-19, having to isolate from our families, friends, coworkers, and dropping activities we enjoy or take for granted like a haircut or a handshake, and important medical visits and procedures we’ve either been delaying or pursuing with extreme concern and extra cautions. As social beings, humans suffer in isolation, and especially our elderly and our youth.
Many of us experienced getting sick with Covid or know someone directly who contracted the disease and may be experiencing lingering effects. 600,000 families in the USA alone lost a loved one to the virus and experienced powerlessness, grief, and the heartbreak of not being able to be with their loved ones, and had to forgo gathering for a memorial service, no hugs, no support, or shoulders to cry on.
We know from research that stress that persists over prolonged periods of time can cause our body-mind to start showing symptoms of discomfort and dis-regulation, which we can interpret as alarm bells. We need to then pay attention and listen to our bodies.
Our response to stress can affect our emotional health and interfere with relationships and normal daily activities, like accomplishing tasks, focusing, making decisions, and remembering. Too much stress can weaken our body’s immune system, increase our risk for physical illness, or make existing medical conditions worse. Prolonged stress can keep cortisol levels high and create inflammation in our tissues and cells, a major culprit in generating disease (Creswell, 2012).
Anxiety can be one of the alarm bells. One might feel worried, afraid, on edge, overwhelmed, or out of control. In the body, it might manifest as a “knot” or tightness in the solar plexus area, shallow breathing, racing heart rate, elevated blood pressure, headache, tight jaw, neck, and/or shoulders.
Or it can show up as anger, irritation, or impatience, often directed outward. Or it might turn inward as feeling sad, down, helpless, or guilty, fatigued, having trouble sleeping. In fact, “fighting” stress can be exhausting and perpetuate the cycle of fatigue and helplessness.
Unchecked or unskilled coping behaviors that might help short term quickly become maladaptive and detrimental if persistent, like overeating or skipping meals, working too much or procrastinating, giving in to passive activities like binge-watching tv, couch-surfing, shopping, to even becoming dependent on smoking, drinking alcohol, or using drugs.
Resilience is innate in human beings, but it needs to be fostered, nurtured, encouraged, and supported; there are many modalities and tools to help us build our resilience muscles, healthy responses to stress, and uplift our spirits short and long term, so we can be also better supporters of others.
As we get to know ourselves, we become aware of less desirable and detrimental states on the onset, and with practice, we can switch to a truly helpful, nurturing mode.
Gratitude – Research shows that practicing gratitude daily creates a positive outlook and benefits our health. We can practice gratitude by identifying and journaling about one positive experience or item to counteract the very natural tendency to pay attention to what is not working, an evolutionary feature of our survival instinct that protects us by alerting us to potentially dangerous situations. A post-it note on the bathroom mirror works too!
Enjoy this 10 min Gratitude meditation:
https://www.mindful.org/a-10-minute-gratitude-practice-to-notice-shift-and-rewire-your-brain/
Mindfulness-Based Stress Reduction / MBSR – a modality which trains us to cultivate present moment awareness in mind and have us tune in to our body sensations. It helps us notice and decrease ruminating, it supports our reframing, our focus on the here and now where we can investigate, accept, make choices and act. Identifying personal strengths and areas of vulnerability can help us be more effective and also recognize when we need to ask for help or get into learning mode.
Yoga and breathwork practiced with skillful guidance can be truly transformative and benefit us in body, mind, and spirit. Simply slowing down our breathing, with even longer exhales, and moving our bodies with the breath shifts us to our parasympathetic nervous system, activates the vagus nerve, lowers our blood pressure, as we journey from anxiety to a more peaceful and healthier state.
Art-making whether it is solo or with other people is a great activity to relax, play, focus, find new ways to see our world, create some distance from a stressful experience, take safe risks, learn to accept, and possibly transform our creation and ourselves in the process.
“It’s important that we share our experiences with other people. Your story will heal you and your story will heal somebody else. When you tell your story, you free yourself and give other people permission to acknowledge their own story.” — Iyanla Vanzant
Through art we have participated and encouraged communities in making colorful banners with uplifting messages to hang outside balconies and windows.
Here is a brief video clip for inspiration: Banners and Flags https://www.youtube.com/watch?v=bf0QtH2ozfo

Move – keep moving in nature whenever possible or at home with plenty of videos and zoom classes, many at no cost. Gardening can be a great way to get your physical activity in nature, uplifting, satisfying, and adding some healthy ingredients to our meals. Even gathering with family and friends via zoom for a meal, or an exercise, yoga, or dance class helps us maintain the camaraderie of the shared experience, plus the endorphins and relaxation. Put on your favorite tunes when doing house chores.
Connections – Use what technology you have available to stay connected to people you care about, and also reach out to neighbors and to the global community; a simple creative idea I learned about has been used during the pandemic in Colombia: in the poorest sections of Bogota, families would hang a red rag or t-shirt outside their doors or windows, to let neighbors and aid workers know they needed help, food, and/or medical care. Very moving and effective.
Nurturing Nutrition – easy gathering ingredients and cooking following recommendations, research, and tasty recipes at Mary Hollander’s Reality-Based Nutrition blog https://www.realitybasednutrition.com/, following Hippocrates’ motto: “Let food be thy medicine and medicine be thy food”.
Kindness – “Be kind whenever possible – it’s always possible”. ~ H.H. The Dalai Lama. A kind act or words that bridge the gap, notice a lovely accessory, acknowledge a positive feature, or make another person feel heard, seen, and validated can change us from the inside out. Include yourself in choosing who to be kind towards 😉
Modalities and Class Resources, safe for cancer patients, are at https://sdcri.org/educational-links/ and www.NancysList.org.
To view and print this article in PDF form click here!
Every Organization Has A Story.
Here’s Ours.
The HeartWay was born out of the work of our Founder and Executive Director Dr. Andrea Deerheart, which encompasses the issues related to optimal wellness of mind, body, and spirit during dying and death–grief and loss, and compassionate, mindful and supportive care. This is her story.
“For over 33 years, I’ve been talking to people about death. I’m often asked “how could you work with the dying?”
My journey on this path began when I was seven. Many family members were dying of heart disease and cancer and I wasn’t allowed to visit them in the hospital or attend the funerals. I can remember my older brother having an accident and I was kept away. I imagined it must be horrific if they wouldn’t even let me see him. I became convinced that illness and death were really, really scary.
I tried to conquer my fear of death by fantasizing what it would be like when I was dead but my imagination only confirmed that death is dark, lonely, scary, and empty. My fear intensified as I grew up and manifested as low-grade anxiety. I lived with the fear the best that I could and pursued my undergraduate studies at San Diego State in marketing and sociology. After what one might call a successful career in marketing for large corporations, I started thinking about getting an MBA. In the meantime, I did everything I could to be safe so that death would not touch me–years of wellness, nutritional studies, vegetarianism, yoga, teaching, and spiritual development followed.
I’ve always wanted to volunteer, to give, and to share with others. My path changed when a dear friend was on the board of directors for a hospice in San Diego county and I asked him if they needed volunteers. Is there a question that one should have significance in the life of someone who is dying – you know, if the door is sprung wide open? So, in I went!
My first person I went to serve who died in my arms changed my life forever. I can still feel that moment, years later. Being present to her death was not at all what I imagined. She slipped away in my arms with a gentle exhalation. I wasn’t scared. I wept and held her. Then I wept some more.
There was no turning back at this moment. I was home. My heart and soul had found a path that filled me with an inner peace I hadn’t yet known in my life. I went back to school, but not for an MBA. I received my first Masters in counseling psychology so I could become a hospice social worker, and upon graduation started working in the hospice system in Orange County. This deepened my connection to the preciousness of life and I love every day. I listened, learned, cared, and became ever more present to death. My fear of death eased and my life became filled with deep heartfelt gratitude.
In the mid-nineties, hospice came under major scrutiny from Medicare and other governing bodies. They became financially dependent on funding to survive and the medicalization (and monetization) of death began. Unfortunately, this detracted from their original mission of providing a holistic approach to end of life which tugged at my heartstrings as I didn’t believe concerns over money should be part of our last breath. It should be a time to say good-bye, love each other, reconcile our relationships, grieve, and honor death.
I’m a strong advocate for hospice services as I believe they are a necessary part of our current medical model of care, but I also believe we have a system that isn’t addressing many of the needs of those facing the end of life. Hearts, desires, and soul yearnings are being untouched, leaving many of the dying alone, fear-laden, shamed, and in an institution in which they may wish not to reside. My deepest vision is that no one dies in unnecessary suffering. I left hospice and continued to do the work that I felt was needed to support those facing the end of life, inclusive of providing compassion, support, education, sanctity, rituals, death with dignity, and love.
My studies advanced to a doctorate degree in mythology and depth psychology. My thesis focused on the cultural, religious, and philosophical practices of death, dying, and beyond. I continued my work as a death doula (someone who cares for the dying, physically, spiritually, and emotionally), advocate, educator, and ordained minister. My practice took me all over the world as I deepened my ability to be present to death. Death is better understood in our psyche and souls when we’re connected to our ancestors in dreams and imagination.
I’ve now held hundreds as they have crossed over the threshold into the unknown. Each person affords me the honor of witnessing a significant piece of the great mystery of this life. The privilege of listening to the echoes of their hearts.
I’ve never charged for my services for those families and loved ones dealing with death. When I’m asked how I can do this work, I answer, “I cannot NOT do this work! The work chose me.” I say this with the deepest of gratitude.
With love from my heart to yours,
Dr. Andrea DeerheartThe HeartWay Executive Director and Founder”
Integrative Oncology Resources and Daily Ritual Summary, Checklist, and Reminders
by Daniel Vicario, M.D.
I’ve had the honor and privilege to work with cancer patients for over 3 decades. During the last few years, I’ve done this as an Integrative Oncologist. I’ve been fortunate to learn so much from them over the years, and I continue to do so with each visit and conversation. I’ve been able to keep a list of tools, empowering and inspiring concepts that continue to evolve. Several of these ideas/experiences I’ve been able to share in the video interviews and as lists of resources detailed in the following summary sheets.
Please share with anyone you believe could benefit from them.
Sending best wishes and blessings to all readers,
Daniel Vicario, M.D.
The following are the Integrative Oncology Resources and Daily Ritual Summary, Checklist, and Reminders lists from Dr. Vicario. Click on the links below for printable PDF versions.
Integrative Oncology Resources
Daily Ritual Summary, Checklist, and Reminders
Integrative Oncology Resources
Here are several recommendations to consider reviewing:
….. 1. Information and resources available on our SDCRI nonprofit website: www.sdcri.org
….. 2. You can watch these three video interviews on Integrative Oncology:
……… a. Conversation with Dr. Paul Mills at UCSD: https://www.uctv.tv/shows/Comprehensive-Cancer-Care-Integrative-Oncology-with-Daniel-Vicario-MD-and-Paul-J-Mills-UC-Wellbeing-Channel-32223
……… b. Conversation with Dr. Mimi Guarneri: https://youtu.be/tjYbLGKIXic
……… c. Zoom video on Friday November 20, 2020 with Dr. Shamini Jain from the Consciousness and Healing Initiative (CHI: www.chi.is). Here is the YouTube link: https://youtu.be/jspzj_T0FqY
………d. Slides shown on the above Zoom video with Dr. Jain from the Consciousness and Healing Initiative: Slide 1 (sdcri.org)
…..3. Educational and inspirational videos on our SDCRI website: https://sdcri.org/edu-art/edu-vids/
…..4. “Commentary on a recent JNCI article about alternative medicine”: https://sdcri.org/edu-art/current-integrative-research-news/commentary-alt-med/
…..5. “INTEGRATIVE MEDICINE” websites:
………a. Academy of Integrative Medicine & Medicine: https://aihm.org
………b. NIH National Center for Complementary and Integrative Health: https://www.nccih.nih.gov
………c. Consciousness and Healing Initiative: https://www.chi.is
………d. T. Colin Campbell Center for Nutrition Studies: https://nutritionstudies.org
………e. UCSD Center of Excellence for Research and Training in Integrative Health: https://medschool.ucsd.edu/som/fmph/research/centers/integrativehealth/pages/default.aspx
………f. UCSD Center for Integrative Medicine: https://medschool.ucsd.edu/som/fmph/research/cim/Pages/default.aspx
………g. UCLA Integrative Medicine Collaborative: https://www.uclahealth.org/integrative-medicine
………h. UCSF Osher Center for Integrative Medicine: https://osher.ucsf.edu
…..6. INTEGRATIVE ONCOLOGY and Integrative Medicine recommended websites:
………a. https://sdcri.org/educational-links/#IntOnc
…..7. Mary Hollander, R.N. nutrition sites:
………a. Mary’s Reality Based Nutrition – San Diego Cancer Research Institute (sdcri.org)
………b. Mary’s Reality Based Nutrition | “Let food be thy medicine and medicine be thy food” Hippocrates
…..8. During challenging moments, you can consider searching online and/or on YouTube meditations with:
………a. Jon Kabat Zinn (founder of mindfulness meditation)
………b. Eckhart Tolle
………c. Belleruth Naparstek
………d. Wayne Dyer, Deepak Chopra and many others you may resonate well
…..9. Nine Surviving and Thriving Beyond Cancer with Belleruth Naparstek: https://youtu.be/9ZnuDXRxYY8
…..10. Deepak Chopra’s YouTube channel: The Chopra Well https://www.youtube.com/channel/UC6d0RMVcoXNCkTpG8PW2dBA
…..11. Deepak interview with Rodrigo Niño on cancer: https://youtu.be/CbdvB3sQjxE
Integrative Oncology
Daily Ritual Summary/Checklist
…..1. Stress management
…..2. Meditation. Visualization. Reflection. Prayer
…..3. Good sleep. Plenty of rest
…..4. Optimizing Nutrition
…..5. Exercise. Yoga. Breathing Techniques
…..6. Honoring our emotions. Allowing them to move through us
…..7. Embracing uncertainty
…..8. Feeling in Control. Empowerment
…..9. Balance. Inner Peace. Homeostasis/Homeo-dynamics
…..10. Grounding. Being in Nature
…..11. Sense of purpose. Gratitude
…..12. Clearing old traumas: ours, our parents, and our ancestor’s traumas that we
carry (epigenetically, etc.)
…..13. Create your own daily “checklist”
REMINDER:
…..• Honor all your feelings
…..• Trust your powerful inner wisdom, your intuition.
…..• Be with those who make you feel good, who support your inner peace in the midst of all the challenges
…..• You are unique. Please do not compare yourself with others
…..• Accept help. You are always giving
…..• See medicines, chemotherapy, surgery, radiation, etc. as Healing treatments, tools in your healing journey
…..• Visualize your potential for infinite possibilities and healing • Message of hope: for any condition considered “incurable” at this time, an answer may be around the corner
…..• Miracles do happen. Spontaneous remissions
11 Questions to Ask About COVID-19 Research
by Jeremy Adam Smith and EMiliana R. Simon-Thomas
How can you tell if a scientific study about the pandemic is valid and useful? We have some tips.
 Debates have raged on social media, around dinner tables, on TV, and in Congress about the science of COVID-19. Is it really worse than the flu? How necessary are lockdowns? Do masks work to prevent infection? What kinds of masks work best? Is the new vaccine safe?
Debates have raged on social media, around dinner tables, on TV, and in Congress about the science of COVID-19. Is it really worse than the flu? How necessary are lockdowns? Do masks work to prevent infection? What kinds of masks work best? Is the new vaccine safe?
You might see friends, relatives, and coworkers offer competing answers, often brandishing studies or citing individual doctors and scientists to support their positions. With so much disagreement—and with such high stakes—how can we use science to make the best decisions?…
… continue reading this article on Berkley’s Greater Good Magazine website!
Medication management for cancer patients and caretakers
by SINGLECARE TEAM, Medically reviewed by GERARDO SISON, PHARM.D.
For cancer patients, medication is a critical aspect of recovery. A patient’s specific mix of medications will be designed in consultation with a care team. Those medications will work best when given at the proper doses and times.
This guide will help cancer patients and caregivers successfully manage the storage, dosage, and special circumstances related to cancer medication.
What are the 5 R’s for medication safety?
Caregivers who follow the 5 Rights of Medication Administration will be the most effective at keeping cancer patients safe and healthy. These are the same steps followed by the care professionals at your clinic or hospital.
- Right drug
- Right dose
- Right time
- Right route
- Right person
Right drug
As you get ready to administer a drug, first make sure you’re using the correct one. Look at the pill bottle, then read the name of the drug out loud.
Right dose
A common cause of dangerous adverse drug events is giving an improper dose. This mistake usually happens when caregivers misread or mismeasure the proper amount.
Right time
A medication plan will only be successful if the proper medication is given at the right time. The best solution is a written medication schedule.
Right route
Cancer medications can be administered as pills, liquids, topical treatments rubbed on the skin, and injectable treatments. Injectable treatments include intravenous (IV) infusions or injections through the vein, intramuscular (IM) injections into the muscle, and subcutaneous (SQ) injections under the skin. Follow the directions given with the medication, and ask for help if you feel you need it.
Right person
Pill bottles can look very similar. As a last step before administering the medication, look again at the medication you’re holding to make sure you’re giving it to the right patient.
General tips for effective cancer medication management
Two important strategies will help you give medication safely throughout the treatment process: keeping a medication list and storing medication properly. Medication storage and handling is especially important because some treatments may be hazardous.
Medication list
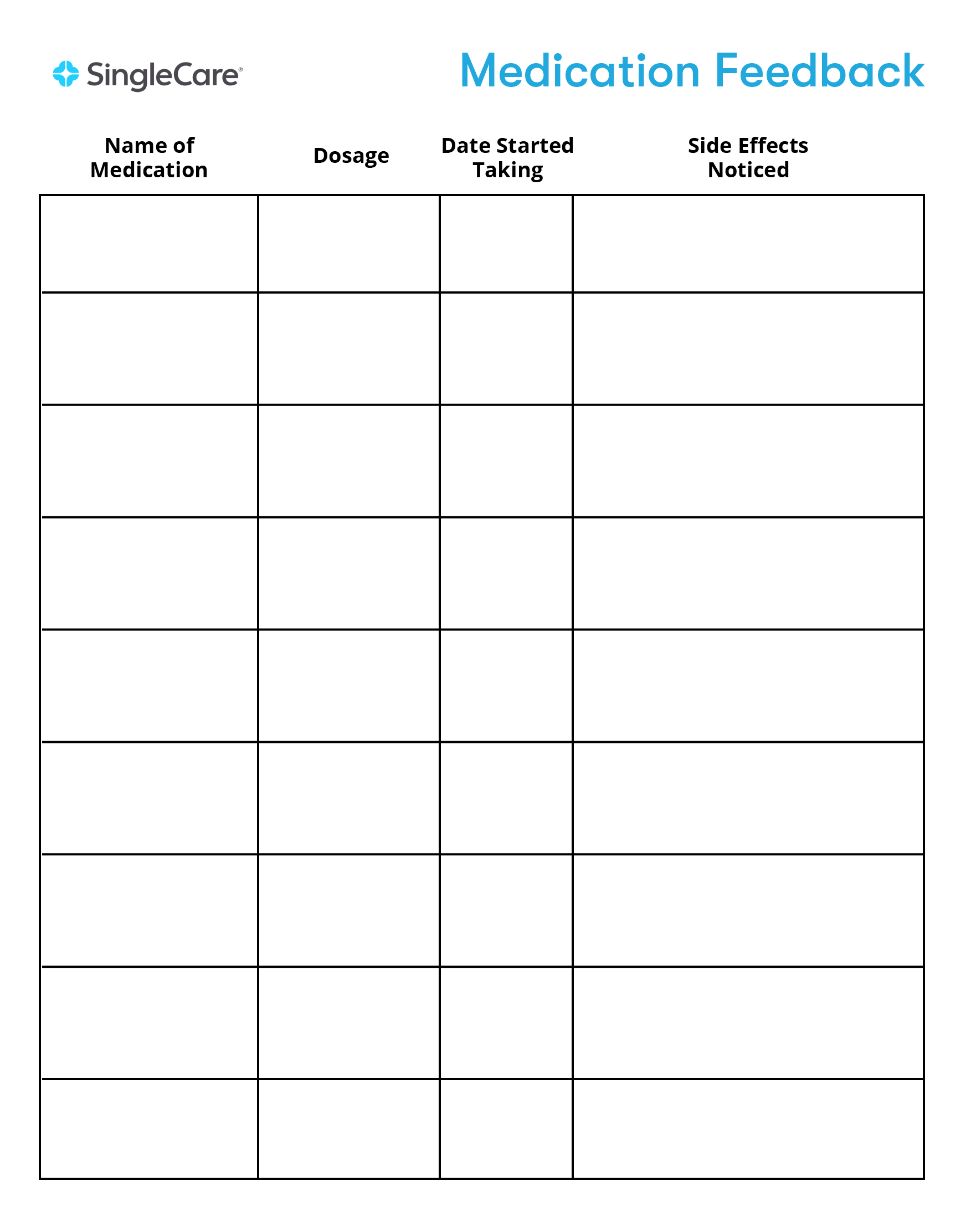
A medication list is a critical document that will be consulted by patients, caregivers, pharmacists, and your doctor. Make sure you add any supplements or over-the-counter medications to the list in addition to prescribed medications.
The medication list should include the name of the medication, the dosage or how the medication is taken, when treatment with the medication began, and any concerns you have such as side effects experienced.

Safe storage and organization
Cancer medications are powerful and very dangerous if taken by the wrong person or handled improperly.
If you have anyone at home who might accidentally ingest them (like a child or pet), make sure to store the pills in a high place they cannot reach. You may also want to invest in a pill lockbox. Never store cancer medications in the bathroom—the humidity can lessen their effectiveness.
Ideally, only the person who is taking the medication will touch it. If a caregiver needs to handle the medication, they should only do so while wearing gloves.
Hazardous at-home medications
If any of the medication being taken at home is hazardous, such as chemotherapy drugs like doxorubicin or vincristine, caregivers will need to take additional safety steps.
Caregivers should be given special kits with instructions and materials for cleaning spills, and special containers for disposing of hazardous medications.
These medications can still be present in dangerous amounts in bodily fluids, such as urine, blood, saliva, etc. If any of these fluids are present on the patient’s bed sheets, towels, or clothes, handle them with disposable medical gloves, and wash the soiled fabrics in hot water separately from other laundry.
The patient should take special care when using the toilet. For 48 hours after an injection or IV treatment, the patient should flush the toilet twice after use, wash their hands well, and cleanse any body parts that have urine or feces on them. The toilet water could still contain trace amounts of hazardous chemicals, so children and pets should be kept away from the bathroom.
Powerful cancer drugs, like any medication, must be taken at the proper time in order to be the most effective. Missing scheduled dosing times completely or taking pills at the wrong time could be dangerous.
To make sure you administer all pills at the proper time, set reminder alarms on an alarm clock or timer. If you have a smartphone, consider using an app designed for medication management.
It’s also a good idea to write down the daily medication plan on a sheet of paper. A physical list can be easily copied and shared with other caregivers and health aides, and you don’t have to worry about phone compatibility or a data outage making the medication plan inaccessible.
Having a record of daily medications is also very helpful at follow-up appointments with the patient’s care team. These appointments are the ideal time to discuss adjustments in medication timing that may help reduce side effects experienced. You may discuss moving the timing of a treatment dose closer to a mealtime, for instance, or further away from bedtime. These are just examples. Never make any changes to a medication plan without first discussing them with the assigned care team.
Understanding the prescription bottle label
Typically, a prescription label has eight parts and types of information. Keep in mind that your own prescription labels may look somewhat different, but they will generally have similar content listed for you to reference. Learn to recognize these parts on your own medications.

- Pharmacy information: Key details about the pharmacy that filled your prescription
- Your information: Contact information of the patient
- Prescribing doctor’s information: Contact information of the physician or healthcare provider
- Drug name and strength: Brand, chemical, or generic name along with the measured amount of one unit of the medicine
- Instructions on taking the medicine: How and when to take the medication
- Prescription information: Specific information to aid in planning for getting refills
- Pharmaceutical manufacturer information: Name of the company that manufactured your medication and a physical description of the drug
- Federal caution statement: Prescription warnings mandated by the U.S. government
Many prescription medications also come with medication guides that are approved by the Federal Drug Administration (FDA). These guides have information about issues specific for particular drugs, and may help patients avoid serious side effects.
At-home injections or intravenous treatment
When it is safe to do so, chemotherapy treatment can be given at home. A home health aide will do the procedure, or train a caregiver to do so.
If a home health aide is administering these treatments at home, they will be responsible for learning about and caring for special equipment, like the tubes, lines, ports, and catheters that are used in cancer treatment. There are many different types. Someone at the cancer care facility will train the home health aide or caregiver about the specific equipment before you start any at-home treatments.
Avoid switching pharmacies or doctors
Cancer treatment is a complex process. The care team will be weighing many factors in developing your medication plan, including your past medical history, allergies, the stage of the cancer, and others.
Because the process is so involved, it’s best to stay consistent with the pharmacy you’re using and the doctors you’re seeing. That means sticking to one pharmacy for all your medications, if possible.
Active treatment and maintenance therapy
Many cancers are treated with the goal of eliminating it from the body. When treatment is in this stage, it is sometimes called active treatment. In a best-case scenario, the patient is completely free from cancer at the end of treatment.
Some cancers are chronic in nature. They cannot be fully cured; they’re only managed with ongoing chemotherapy to keep the cancer from spreading or worsening. Such cancers may include ovarian cancer, some leukemias, and some lymphomas.
Once treatment has successfully reduced the signs and symptoms of the cancer, the disease is said to be in remission. When the cancer isn’t growing, it may be called “controlled” or “stable.” Growing cancers are often described as in the progression phase. If a chronic cancer begins progressing, you will likely have to resume treatment.
Homeopathic, alternative, or complementary cancer treatment
Hospitals and cancer care facilities take an evidence-based approach to treatment. The cancer treatments recommended by your doctor have proven effective in clinical trials of cancer patients.
There are other treatments that are not proven to eliminate cancer, but can relieve some symptoms of the disease. Meditation may help reduce anxiety. Tea may assist digestion or reduce nausea. Massage or acupuncture may relieve pain. Many cancer treatment professionals encourage the use of these therapies when used in conjunction with evidence-based treatments.
Side effects
The side effects of cancer treatment can affect a patient’s ability to stick to their medication plan. For example, confusion or delirium is a serious side effect associated with cancer treatments and pain-relieving drugs. Less serious cognitive lapses during cancer treatment—like forgetting names or dates, or a general feeling of mental cloudiness—are sometimes called “chemo brain.” A patient who isn’t thinking clearly may have a harder-than-usual time remembering to take medication.
Chemotherapy can affect the entire body. Common side effects of cancer treatment include general fatigue, hair loss, constipation, diarrhea, and mouth sores, among others. Other side effects, such as nausea, taste and smell changes, and difficulty swallowing, can make taking medication unpleasant.
Discuss side effects with your care team. If side effects are so severe that the patient can no longer safely take their medication, adjustments to the dose or type of medication can be made.
When to immediately contact your medical team
During most cancer treatments, the patient spends the majority of their time at home. Many medical issues that happen at home can be handled by the caretaker or the patient themselves. But if any of these events occur, reach out to your care team.

-
- You need a refill of your medication
- You lose, spill, or vomit a dose
- Someone else accidentally takes the cancer patient’s medication
- Any redness, warmth, swelling, damage, or pain at the port or injection site
- Fever
- Patient can’t take treatment or refuses treatment
- Signs of an allergic reaction to the medication
Safe disposal of cancer-related treatments
With any medication, safe disposal is important. Medications are powerful chemicals that are dangerous if accidentally ingested, or if they get into the soil or groundwater.
Cancer medications are often extremely hazardous. Your care team should give you specific instructions for disposing of these medicines safely if they’re no longer needed. You may also get special equipment like a biohazard container. You should not try to figure out how to dispose of a cancer medication. If you weren’t given specific instructions or don’t remember what the instructions were, call your care team and ask for help.
Cancer is scary, but medication management doesn’t have to be
Aggressive cancer treatment can be a life-altering experience. Pills, needles, and intravenous tubes may temporarily become as regular a part of your life as the daily mail. For caretakers, you’ll be assuming a new role as a part-time nurse. But you have a team of dedicated, full-time medical professionals behind you. They will help you figure out the best home treatment plan for you based on your availability and skills. Educate yourself by reading guides like this one, but don’t hesitate to ask for help. You can do this.
Check out the original article and the webpage here.
Hope Made Visible™, International
An ongoing journey of healing, compassion, and resilience.
by Alessandra Colfi, PhD

“Only through our connectedness to
others can we really know and enhance self.
And only through working on the self
can we begin to enhance
our connectedness to others”.
— Harriet Goldhor Lerner
Hope Made Visible™, San Diego Cancer Research Institute’s global expressive arts initiative, has received even greater attention since the whole world turned upside down, and outside-in, because of the COVID-19 pandemic. More than ever people have been seeking creative ways to stay connected and feel the support of community while physically distanced and only able to see each other’s eyes in public. Especially for our vulnerable cancer survivors and their families, the elderly or those who live alone, the isolation can be particularly grueling; no hugs, no shaking hands, no getting together for workshops, no group activities, limited travels are taking a toll as we approach the 8-month mark and likely expect prolonged social distancing recommendations will remain in place next year.
The pandemic added a thick layer of anxiety, lack of freedom, irritability, and fatigue to those affected by cancer; patients have been expressing that their view of cancer as the most serious, life-altering experience they could ever experience evolved into a whole new level of emotional and mental stress. More than ever-supportive services, coping skills, and resilience through meaningful engagement need to be enhanced, especially in the prolonged quarantine.
Not only at this time it has been difficult to create a new sense of ‘normal’, but it hit especially hard those who lost loved ones and have been struggling with not been physically present with their loved ones at the end of their lives and gathering with family and friends for the very necessary, soulful rituals of celebrating and remembering their precious lives and relationships.
How do we deal with the heaviness of this time? How do we keep going when so much of our lives is so hard, sad, uncertain, and unpredictable? How do we breathe through the anguish and find joy and gratitude in being alive?
My answer is: community and the arts! Here is a short list of benefits based on extensive research and narrative accounts by participants:
- Art fills occupational voids, distracts thoughts of illness
- Improved well-being by decreasing negative emotions and increasing positive ones
- Improved medical outcomes, trends toward reduced depression
- Reductions in stress and anxiety; increases in positive emotions
- Reductions in distress and loneliness
- Increase in compassion for others
- Improvements in flow and spontaneity, expression of grief, positive identity, and social networks
And here comes Zoom, our ubiquitous virtual meeting platform.
I facilitated Hope Made Visible™ workshop series during the summer for cancer patients and vulnerable community members through UC San Diego Health; with geographical boundaries evaporating thanks to the virtual delivery mode, patients from all over the country joined in, creating additional interest and new personal connections and exchanges.
We have been working together with reminders, tools, mindful attention, and processes that offer a pathway to authentic artistic expression. There is no better time to delve into the depths of ourselves in a safe, supportive group, to explore and express how we feel, and to bear witness to these discoveries with acceptance, in simple accessible ways.

Pre-Covid group workshop

Since 2012 we have collected more than 1,500 unique Hope Made Visible™ flags created by cancer patients and families/friends from all over the world. They are currently displayed as a powerful, moving exhibition at California State University San Marcos ~ Kellogg Library until December 31, 2020.
Now more than ever these soulful flags touch and inspire all of us with hope, connections, and compassion. I cannot wait to read and share thoughts and comments left by visitors in our guest book!
SDCRI has been collaborating with highly respected organizations and practitioners through the years; one of those collaborations in 2015 and 2016 was with Habitat for Humanity in Los Angeles / San Fernando Valley, which focused on Hope Made Visible™ flag making workshops and more Expressive Arts with Veterans transitioning from homelessness, addiction recovery, PTSD.
A new opportunity for Hope Made Visible™ opened up to reach out to the public with the intention of bringing solace and healing, upon invitation by The HeartWay to collaborate at an Expressive Arts initiative to offer Healing Grief Thru HeArt live online sessions to individuals and family who lost loved ones during the pandemic and/or are feeling the psychosocial/emotional toll of the pandemic, as we recognize the experience of PTSD or even Ongoing Traumatic Stress (OTS).
In this challenging time, we want to support those who are grieving, especially if in isolation, and experiencing complex emotions. It is important in order to feel supported and promote healing to validate one’s unique experience, stay connected, and allow grief to be expressed thru a compassionate, safe, non-judgmental medium like simple hands-on art, and share it with others in our virtual community. By giving ourselves permission to create art, by tapping into awe, wonder, and beauty, we invite healing and create potentially transformational shifts.

Art has the Power to Heal Humanity
This new collaboration would start with a hands-on expressive arts workshop via zoom on October 24th; the presentation includes a brief history and inspiration slides featuring special moments involving Hope Made Visible™ and Healing Grief Thru Heart: https://www.youtube.com/watch?v=pBcm1s7wnko
Everyone will be invited and guided through a process to create a flag in remembrance and celebration of the family member or friend they lost, with the opportunity to send the flag to us, to join the growing global initiative, and become part of a future public exhibition.
Participants will also be invited to create larger banners on their own, which individuals and families can hang from their windows or balconies, fostering community connections and solidarity.
Banners and flags have been used throughout history, across cultures and traditions, to symbolically honor the death of a loved one, to express compassion and to enhance healing through individual and collective participation. Our intention is that through cooperation, participation, and HeArt centered creativity, we will inspire a cultural shift to emerge around a community-centered approach to grief and loss.
Our goal with this new collaboration is to gather an additional 1,000 Flags and 500 Banners, as an ongoing opportunity.
How to participate?
RSVP: Please email Alessandra Colfi, PhD at Alessandra@AlessandraColfi.com or text 858.735.5708. We will then send you the Zoom link to join us on Oct. 24th!
ADDITIONAL INFO:
1) You do not need to be an artist to participate — your personal style and creativity is welcomed!
2) Materials:
– Blank paper
– White or off-white fabric cut in 6” X 10” sections for each Flag
– A paper grocery bag (cut open) or pillowcase for each Banner
– Markers, oil pastels or crayons, acrylic paints, tempera, a paintbrush
– Optional: glitter, embellishments such as buttons, jewels, beads, ribbon, trims, stamps, quotes, natural findings like pods, leaves, twigs.
I am deeply grateful to continue this journey of empathy, hope, compassion, resilience, and community. In closing, enjoy a poem by storyteller, film maker, and poet Nic Askew as a thoughtful and comforting reminder:
THE ADVENTURE OF UNCERTAINTY
There Was A Time When
I Looked For Certainty.
Certainty In The
Outcome Of
The Events Of
My Own Life.
And Then I Realized
That There Was
Only One Certainty.
And That Was
That It’s All OK.
That There’s Something
That Could Never Die.
And Now I Realize That
The Total Uncertainty
Of The Events Of Life
Is The Adventure.
And That’s The Wonder. ~ Nic Askew
Namaste,
Alessandra
Breathe Away Anxiety
by Lisa Nicholson
 Last week in our breast cancer support group, we talked a lot about anxiety. How it comes up before scans and procedures. How it sneaks into our bedrooms at night and keeps us awake.
Last week in our breast cancer support group, we talked a lot about anxiety. How it comes up before scans and procedures. How it sneaks into our bedrooms at night and keeps us awake.
Here’s a quick and effective tool for taking anxiety down a few notches. Is it as effective as Atavan? Probably not. But anything which takes the edge off that awful feeling is worth a try.
The technique is called “4-7-8 Breathing”, made famous by Dr. Andrew Weil.
Here’s how you do it:
- Sit or lie down in a comfortable position.
- Inhale slowly through your nose for a count of 4.
- Hold your breath in for a count of 7.
- Then exhale through your mouth with a “whoosh” sound for a count of 8.
- Repeat this cycle for at least 5 breaths.
 For a more “advanced” technique, you can hold for a count of 7 after the exhale before inhaling through the nose for the next round.
For a more “advanced” technique, you can hold for a count of 7 after the exhale before inhaling through the nose for the next round.
Why does it work? Our nervous systems can’t be in “fight or flight” and “rest and digest” at the same time. When we feel anxious, our sympathetic nervous system is preparing us to run for our lives. We have tons of energy for a quick burst allowing us to sprint to safety or climb a tree or run into a burning building to save a puppy. The nervous system can’t tell whether the “danger” is a thought in our head or a true threat to our bodies so it reacts the same way to both, giving us that feeling of needing to run screaming from the room along with palpitations, cold sweat, shortness of breath, dilated pupils…you KNOW because we’ve all been there.
What we need to do is “flip the switch” to the part of the nervous system which has us feeling warm and cozy in our safe nest, allowing us to rest and digest – the parasympathetic nervous system.
Slowing down the breath and especially pausing the breath temporarily increases the carbon dioxide in our bloodstream and calms the nervous system. The sighing “whoosh” exhale empties out more of the air from our lungs than we usually do, and the vacuum created allows the next inhale to go deeper which brings more oxygen in. It also tricks the brain into letting go of the need to run for our lives and gives our thoughts a chance to catch up to our physical reaction. The result – a quick and easy way to at least temporarily calm our nervous systems and reduce that feeling of anxiety.
And for an added bonus, there are no chemicals, no interactions to worry about with chemo or radiation, and you can use this technique as often as you want with no consequence except a calmer nervous system.
Here’s a link to Dr. Weil demonstrating how to preform this breath.
For more about the power of breathing consciously, check out Breath: The New Science of a Lost Art by James Nestor. It’s just one of the books I’ve been reading this summer, and there are some great information and techniques there.
Travel during the COVID-19 Pandemic
from cdc.gov
This holiday weekend, and in the holiday season to come it is extremely important for everyone to be mindful of virus-etiquette while travelling. Cancer patients and healthy people alike are at risk, and need to be concerned for themselves, as well as for their loved ones.
This month in Featured Articles we would like to focus on a piece that is centered around traveling with the pandemic in mind, posted on the CDC’s website. Here is an excerpt below, but please follow the link and lear nmore.
Protect yourself! Protect your loved ones! Protect everyone around you!

Travel increases your chances of getting and spreading COVID-19. Your chances of getting COVID-19 while traveling also depend on whether you and those around you take steps to protect yourself and others, such as wearing masks and staying 6 feet away from people outside your household (social distancing). Airports, bus stations, train stations, and rest stops are all places travelers can be exposed to the virus in the air and on surfaces. These are also places where it can be hard to social distance. In general, the longer you are around a person with COVID-19, the more likely you are to get infected.
Continue reading here!
Cold Flashes and Breast Cancer
by Lisa Nicholson
Yes, COLD FLASHES are a thing! In our Breast Cancer Support Group, we recently talked a lot about thermal dysregulation – all the weird body temperature stuff which comes with menopause whether “natural” or from hormone suppression. One of our members was having chills and goosebumps. She had a full lab workup to figure out what was going on which turned up exactly NOTHING.
I did a bit of research and discovered that cold flashes are actually well documented, especially among breast cancer survivors. Nobody knows exactly why they happen – while there has been a ton of research on the mechanism for HOT flashes, cold flashes haven’t been studied.
Hormone fluctuations of perimenopause, stress, and inflammation can all affect the temperature control center in the brain – the hypothalamus. When the brain gets a signal that the body is too warm, the hypothalamus will drop the temperature a bit. When you’re not REALLY too warm, this will make you feel instantly chilled. Same thing happens with a hot flash, in reverse. The brain gets a signal that the body is chilling, and the hypothalamus sends out a signal to increase the body temperature and send extra blood out to the surface of the skin to warm you up, making you feel hot.
Nobody really knows why we get incorrect temperature signals to the brain. I’ve joked with my husband that my thermostat needs replacing, and while that’s great for humor, we don’t know how to fix a human’s thermostat.
Here’s what the research says:
- women on hormone suppression (tamoxifen, aromasin, arimidex, letrazol, etc.) who experience hot flashes tend to have fewer recurrences of cancer than those who don’t
- estrogen plays a role in dilation of blood vessels, especially at the surface of the body, so lower estrogen levels (or no estrogen) likely have an effect on the body’s ability to regulate temperature through dilating/constricting vessels in the skin
- it appears that the sensation of cold is NOT related to hormone regulation in breast cancer patients) sensation of cold is described in many cancer patients, not just breast cancer patients, and lasts beyond treatment for some patients
- mechanisms being explored include hypoglycemia (low blood sugar), inadequate protein intake, anxiety, environmental stress, dehydration, exposure to toxins such as nickel or cadmium, and chronic low-grade infection
Here’s a link to the article I read in case you want more than my summary – it’s medical research, so be prepared for some Medical-ese. 🙂
Other reasons for chills (besides a fever!) include:
- panic attacks/anxiety
- malnutrition
- hypothyroidism (including cases where the thyroid numbers are in the low range of normal)
- hypoglycemia
- actually being too cold or exposure to cold
“Goosebumps” are typically a sign of sympathetic nervous system activation, and they may or may not come with a feeling of being chilled. When you’re too cold, the hair follicles contract to raise the hairs on your body as an extra layer of insulation. But this can also happen when you’re anxious, afraid, excited, or even sexually aroused.
So feeling chilled plus goose-bumps in absence of exposure to cold is most likely due to either dietary stress (low blood sugar, dehydration, or low protein intake) OR a sympathetic response due to anxiety or agitation.
I always recommend that if you are having weird symptoms you can’t explain that you make sure your oncologist knows about it. If you’re having cold flashes please consult with your physician to be sure there’s nothing serious going on! Once you’re medically cleared, try increasing your water intake, making sure you eat a good blend of protein and complex carbohydrates throughout the day so your blood sugar remains level (consult a qualified nutritionist if you don’t know how to do this), and using your tools for managing stress. Acupuncture, massage, neurofeedback, biofeedback, and psychotherapy can all be helpful tools for balancing the sympathetic nervous system and relieving anxiety.
Depression in the time of Covid-19
by Paul Brenner, M.D., Ph.D.
I have been lying around for the past few years as a result of the neuropathic pain of my lower extremities. To begin with, the pain should have been enough to cause depression. For some reason, depression never took hold. For some mystical, magical reason, during the isolation period of our pandemic, my neuropathic pain has slowly diminished. As a result, I have become more mobile and with mobility, I find myself depressed.
Depression has been a foreign emotion in my life up until now. I’ve been aware of this emotion in others but never within myself. With most of my pain being absent, I thought that I would have been ecstatic, but I’ve been amazed that rather than elation, I’m finding myself stuck in a depressive state. So as anyone finding themselves in such a state, I thought that this would be the time for self-analysis.
Why depression now, instead of exaltation for not having the excruciating pain of electrical shocks raging through my legs and intermittently invading my days and nights. In searching through the dusty- attics of my mind, I experienced my first “ah-ha” in a long time. My father owned a bar in Brooklyn since prohibition. He was one tough son of a bitch. How we dealt with pain always elicited a story from my Dad about Brooklynn at the turn of the early nineteenth century. When he was a kid and a young adult, bravery was the Hallmark of survival. The gangs of Brooklyn and New York’s East Side were raging as was bootlegging. Toughness and street smarts were essential for survival, not school. For me, as well as my two sisters, how we dealt with our everyday cuts and bruises were the key to my father’s love or disdain. Admitting to discomfort was the last thing the Brenner kids allowed themselves to experience.
That bit of self-analysis has paid off. When I experienced what I have called “excruciating pain,”
I did not smile through it, although it never lasted for more than 3-4 minutes. Yes, I would scream from the sudden, sporadic pain. It always caught me unexpectedly. Pulling back my emotions into some deep hidden place, I would quickly get back to whatever I was doing, simply saying “it’s over, it’s over.” And quickly resumed some insane task as if nothing occurred. There is no question that I was embarrassed about the scream and wanted to cover it up as soon as I could.
But why the depression now that I had minimal pain. As a result of analyzing my childhood, this also became obvious. Along with pain, I had lost the mobility of my lower extremities. The immobility was not only the result of the neuropathic pain but the weakness of my pelvis and hip muscles. I had multiple fractures of all my hip bones due to prostate cancer and demineralization of most of my bones as a result of the hormonal blockade of testosterone to treat my prostate cancer from reoccurring. I was a mess. But in spite of that fact, I was now able to walk a little with a walker. So, Paul, now that you can walk with a walker farther than laying around in a Lazy Boy, I could walk around the apartment with minimal discomfort. I could now accomplish so much more with my walker. Now there are no excuses for living the way I had been living. “Get out and do something!” My inner voice cheered me on. As a child, teenager, or adult there was no way I could just sit around and not accomplish something. My previous reason for having pain and an inability to walk was at first difficult but in time, I just rested into it. This took a while to achieve because, in my life, rest was never an option.
Now back to Covid-19 and the “new me” in spite of being 87 years old. There really aren’t that many things to do with the “Stay at home! Six feet distancing! Masks! Gloves and hot water dictums. Now I’m also thinking to myself, I can barely walk, by the time I usually get to the entrance of our building, l am exhausted. I always have to turn around. I typically re-enter the apartment, barely get to the lazy boy and pass out, berating myself for not being able to walk farther. I just realized “father “and “farther” are not only close in sound but are close in meaning. Most fathers, the moment they see their child, whether it be in the delivery or waiting room, suddenly become the chosen provider and are driven to achieve more than they ever believed possible. The need to go further in their career now as his provider becomes ignited within moments of seeing their newborn. This brought to mind the quote by Robert Browning, “man’s reach should exceed his grasp”. This nineteenth-century dictum can be an unconscious driving force for so many of us. If we are not doing something when that something “should” be done or the thought of achieving arises, so many of us dealing with Covid-19 enter variable states of depression.
So, I ask all those who may be reading this article, to give yourself a break. Enjoy a break from achieving, doing, and think about how your childhood shaped your life, your emotions.
How Meditation Can Support Your Community and Wellbeing
by Nina Fry-Kizler, MA
 We often think of the nervous system as a single structure regulating our body. However, our nervous system has two very different parts, the sympathetic and the parasympathetic. In these stressful times, understanding how our bodies respond to stress, how stress affects our immunity, and the interaction between the two is vital for optimal health.
We often think of the nervous system as a single structure regulating our body. However, our nervous system has two very different parts, the sympathetic and the parasympathetic. In these stressful times, understanding how our bodies respond to stress, how stress affects our immunity, and the interaction between the two is vital for optimal health.
The human nervous system’s immediate response to stress is based on an animal-like instinct. However, we differ from animals because we have the capacity for meta-cognition — we are conscious and also aware of our consciousness. We have the capacity to reflect on things that we think and feel, which is an important component in managing our stress response.
Our stress response is hard-wired into our nervous system, built into our DNA to enable our survival when we were being chased by a hungry lion. Today, that same hard-wired response is triggered when we are in major physical danger. When we experience stress of this kind, the sympathetic nervous system kicks into gear and does things like increasing our heart rate, dilating our pupils, causing our breath to quicken, and pumping oxygen to muscles that would be needed to flee to survive. To have the energy and resources for all of those important processes, the body shuts down other systems that are not considered critical during a major physical threat, such as digestion, reproduction, and immunity.
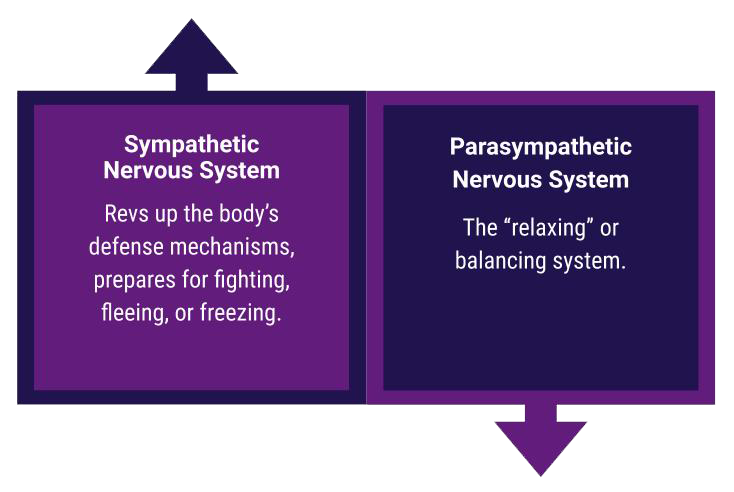 Here’s where things get interesting… Nowadays, few people are faced with that intense kind of physical danger, but our stress response will still kick into gear when we have what’s called a “perceived” stressor, like a tight deadline at work, an argument with a loved one, or a fast moving pandemic that has uprooted our lives. Even if we aren’t being impacted directly, our mind can conjure up many different frightening scenarios as to how we (or people we love) might be impacted. Our sympathetic nervous system cannot tell the difference between an actual physical threat and an imagined or perceived threat and it will marshal all the same resources and turn on the same physiological systems even when we aren’t in actual physical danger.
Here’s where things get interesting… Nowadays, few people are faced with that intense kind of physical danger, but our stress response will still kick into gear when we have what’s called a “perceived” stressor, like a tight deadline at work, an argument with a loved one, or a fast moving pandemic that has uprooted our lives. Even if we aren’t being impacted directly, our mind can conjure up many different frightening scenarios as to how we (or people we love) might be impacted. Our sympathetic nervous system cannot tell the difference between an actual physical threat and an imagined or perceived threat and it will marshal all the same resources and turn on the same physiological systems even when we aren’t in actual physical danger.
The good news is that our parasympathetic nervous system counterbalances the response of the sympathetic nervous system by managing relaxation, rest, re-building, and the optimal functioning of our immune system. The even better news is that because of our capacity for meta-cognition, if we realize we are in a stress response and we are not in actual immediate physical danger, we can consciously choose to intervene in that process and switch over from a sympathetic response to a parasympathetic response. When our body is in the parasympathetic state, it directs energy towards supporting systems like digestion, reproduction, and immunity. When we take time to consciously relax, our bodies release muscle tension, lower blood pressure, slow the heart and breath rates, and reduce hormones like cortisol (aka – the “stress hormone”).
As a teacher of mind-body medicine for stress reduction and boosting health and well-being, in times like these, I don’t see relaxation or self-care as luxuries; I view them as crucial ways to support our immunity and our health.
How do you help your body switch over to the parasympathetic nervous system and support your immune system to be strong and fully functional? Meditation is an incredibly powerful tool for this. At IONS, we have conducted research on how meditation helps support people’s health in a variety of populations and health conditions, including reducing the stress response, cortisol, and glucose intolerance in pregnant women in our study Effects of a Mindfulness-Based Intervention on Distress, Weight Gain, and Glucose Control for Pregnant Low-Income Women. We recently completed research phases in two of our studies on the impact of meditation on depression and anxiety symptoms in older adults: iRest (Integrative Restoration) Meditation for Older Adults with Depression Symptoms and Internet Mindfulness Meditation Intervention (IMMI) Improves Depression Symptoms in Older Adults (for all of the papers published on these studies, see the Additional IONS Research section below). Our Director of Research, Dr. Helané Wahbeh has also published a systematic review on Mind-Body Medicine and Immune System Outcomes.
Dr. Wahbeh, who is also a naturopathic physician, is a very skilled meditation facilitator. Try out the short (8 minute) meditation that she recorded at a recent Noetic Global Gathering which specifically guides you into a meditative state that supports your immune system. Additionally, we just completed a free online ConnectIONS Live: Noetic Approaches to Health & Wellbeing webinar that featured experts in the field of noetics discussing ways to support your health and well-being, which also includes additional meditations.
Additional IONS Research
iRest (Integrative Restoration) Study
· iRest Meditation for Older Adults with Depression Symptoms: A Pilot Study
IMMI (Internet Mindfulness Meditation) Study
· Internet Mindfulness Meditation Intervention for the General Public: Pilot Randomized Controlled Trial
· Internet Mindfulness Meditation for Cognition and Mood in Older Adults: A Pilot Study
The Queen of Pandemics: Corona virus reflection and resources
by Alessandra Colfi, PhD, RYT-200, ZIN®
I have been pausing and reflecting on what this pandemic is teaching us. I’m sure I’m not alone in considering this as Nature’s wake-up call to our complacent civilization, to our interconnected lives across the planet, bringing in focus kindness, compassion, and our great responsibility towards one another and Mother Earth.
Flexibility and curiosity are key to resilience, as we shelter at home, restructure our daily lives, morph our work and community to online platforms when possible, as we improvise and creatively problem solve, offer support for those who are sick, homeless, vulnerable, and find quiet moments to recharge and renew.
It’s not easy to keep up with (and often to tune out) the immense amount of content out there from the news outlets to the online resources and groups that are flooding our inboxes daily.
A silver lining? The air and water are cleaner than ever since fewer cars and trucks travel on our streets and freeways. I’ve been pleasantly surprised by a peaceful silence more often than expected.
While it’s been very difficult to suspend in-person classes and programs, and lose sources of income – hopefully temporarily, our community has stepped up in a big way. Here are a few trusted community resources to keep you connected, engaged, inspired, and moving!
-The Center for Mindfulness at UC San Diego Department of Family Medicine and Public Health offers free Mindfulness Resources like guided audio & video sessions in English and other languages here: https://medschool.ucsd.edu/som/fmph/research/mindfulness/mindfulness-resources/Pages/default.aspx
-North County Cancer Fitness transitioned to online ‘live’ classes through Zoom; if you are not on the mailing list, visit the website www.NorthCountyCancerFitness.org and sign up for free. Download the free App at www.zoom.us and when you receive the notification, click on the link to join a class like Gentle Fitness, Gentle Zumba, Gentle Yoga, or Gentle Kick Boxing.
-In addition, to live classes, you can follow my Zumba routines at your leisure on YouTube. Feel free to contact me for free zoom classes like Zoomba on Sundays and more Yoga: Alessandra@AlessandraColfi.com .
-Be Well has made several Yoga for Cancer Recovery Classes available online, adding co-founders Mary Baker and Heidi Borsch YouTube videos for specific topics. Visit www.BeWellTherapy.net
If you feel called to donate online, donations are always welcome and appreciated.
My Expressive Arts program will soon be available ‘live’ via zoom through UC San Diego Health – stay tuned!
 In the meantime, play with a nature-based art project, suggested by one of my dedicated artists: Make a Flower Mandala arranging leaves petals and pods collected in the garden or on a walk as you get your much-needed dose of Vitamin N! Remember to take a picture when you complete each one and feel free to share.
In the meantime, play with a nature-based art project, suggested by one of my dedicated artists: Make a Flower Mandala arranging leaves petals and pods collected in the garden or on a walk as you get your much-needed dose of Vitamin N! Remember to take a picture when you complete each one and feel free to share.
-Emotional Freedom Technique is a very useful tool that can be easily learned and practiced for a few minutes to help lower stress and anxiety: https://eft.mercola.com/
Research shows that yoga, meditation, moving, cultivating curiosity and mindfulness practices help our minds and bodies cope with stress and anxiety, strengthen the immune system, keeping us healthier and more present and connected, with compassion and gratitude.

Best Essential Oil Brands Based on In-Depth Reviews
from ConsumerAdvocate.org

Essential Oils can be an excellent tool for improving your physical and emotional health, or even just to change the mood of your day. From incense oils and perfumes to soaps and lotions, or even the occasional ingestible supplements (taken only as directed by a healthcare professional). However you like your oils, it is vitally important to know what is in them. Not all manufacturers have your health in mind, or the health of the planet for that matter.
Consumer Advocate recently ran an in-depth study on several popular essential oil brands. They checked into quality, safety, sustainable sourcing, and educational information offered to consumers by each company:
 “With so many essential oil brands out there, it can be hard to find the right one for you. Instead of a top ten list of the best essential oil companies, we took an in-depth look into the industry by reviewing 11 well-known brands.”
“With so many essential oil brands out there, it can be hard to find the right one for you. Instead of a top ten list of the best essential oil companies, we took an in-depth look into the industry by reviewing 11 well-known brands.”
Don’t just exercise caution in how you use your oil. Keeping track of what’s in your oil, or what it’s production does to the environment should be deciding factors as well.
Head to their page now for more on what their team of researchers has uncovered for us.
Featured Articles Archive 2019
Featured Articles Archive 2014-2016
Featured Articles Archive 2017-2018